by Rahul Goswami
Introduction
The skin is the largest organ in the body. Its physiological purpose is to protect the body contents from foreign pathogens and maintain thermoregulation.
The skin layers consist of:
- Epidermis – outermost layer containing epithelial cells
- Dermis – middle thicker layer comprising connective tissue, nerve endings, blood vessels and sweat glands.
- Subcutaneous tissue – lies just above the muscle layer and contains fat cells and connective tissue.
Damage to the skin can be temporary or permanent, and a common mechanism is burns. This chapter will look at the different types of mechanisms along with their assessment and management.
Thermal Burns
When excessive heat is applied to the skin, the destruction of the tissue is known as a thermal burn. This may involve inflammation and healing but if enough heat is applied, there is coagulative necrosis and that area of skin is dead. The type of burn depends on many factors and only careful assessment with appropriate treatment can lead to good outcomes.
Assessment
- Depth
- How deep the injury is can be estimated from the surface condition as well as the mechanism.
Burn Degrees
| Degree | Examination findings of skin | Example |
|---|---|---|
| 1st degree or superficial | Red, painful | Sunburn |
| 2nd degree is divided into: - superficial partial thickness - deep partial thickness | Sometimes blistered, painful, moist | Scald or flash burn |
| 3rd degree or full thickness | Dry, white, insensate, leathery and decreased sensation | Flame or immersion |
| 4th degree or deep full thickness | Damage extends to fat, muscle or bone | Chemical or electrical |
- Area
- The area affected is a good predictor of outcomes. Here is a calculator to remind you of the importance of surface area burnt for survival. Most calculators are only applied to 2nd and 3rd-degree burns.
- Estimation of the area can be done in the following ways:
- Rule of Nines.
- Palm area estimation – This utilizes the fact that the palm (including fingers) of patients is approximately 1% of the patient’s body surface area. Estimate how many “palms” is burnt to get the approximate total burn surface area % (or TBSA). This is especially useful in children.
- Pediatric assessment is more difficult as their surface area is unlike adults. This link is helpful.
- Location
- certain areas of the body are more susceptible to edema and constriction and hence aggressive management is warranted. Examples include:
- Genital burns – fertility consequences
- Facial burns – cosmetic and psychological sequelae
- Ocular burns – lasting visual impairment
- Airway burns or inhalational burns – this requires eventual airway protection as the swelling will occlude the ability to breathe in a few hours
- Special consideration in the assessment of burns in children must be given to Non-Accidental Injury (NAI) or child abuse. Certain patterns of burns are suspicious in nature and if seen, should alert the physician to the safety of the child. Examples of these patterns include:
- Glove or stocking distribution indicating forced immersion
- Cigarette marks or other implement contact marks
- certain areas of the body are more susceptible to edema and constriction and hence aggressive management is warranted. Examples include:
Management
- First aid – the primary treatment is cooling the burn area with running water. This not only gives pain relief but also halts the thermal coagulative process and prevents more area of skin being damaged. Following this, burns should generally be wrapped in dry cling film or dressing before transport to a medical facility. This reduces pain from surrounding clothes and wind. The author was once asked to explain minor injuries including burns and below is the video for it:
- Analgesia – simple oral analgesia (paracetamol or NSAID) followed by opioids if need be. This is the most important step in hospital. Below is a good video for the different types of treatments, applications, and dressings available.
- Fluids – When skin is lost, a large amount of fluids may leak into the injured space and also evaporate. Regimens may vary but a good rule to follow is the Parkland formula. Here is an online calculator for this. In essence, give in mls:
- 4 x weight of patient x TBSA burnt (%)
- Give 1/2 of the total in 1st 8 hours, and then give 2nd half over next 16 hours
- Hartmann’s solution is the ideal replacement fluid
- Pediatric patients require even more specific control of fluid replacement and have their own formulae.
- Specific dressings and burns ointments have changed over the last decade. Here’s a good, updated site for such information.
- Blister management – whether to remove or puncture the blister or leave it alone has been controversial for a long time. The current consensus is to de-roof them.
- ATT – Anti-tetanus toxoid for anyone not immunized or whose last dose was more than 10 years ago.
Referral to the Burn Unit
The burn unit is a specialized unit which deals specifically with burns patients’ needs (dressing changes, escharotomy, debridement, physio, etc.). They are essential units which provide specialist care and dedicated rehabilitation.
Criteria for referral vary between countries but in general patients who require referral or review include:
- Total Burn Surface Area (TBSA) greater than 10% in adults
- TBSA greater than 5% in children
- Full thickness burns of any area
- Circumferential burns of limbs or chest/abdomen
- Facial burns or inhalational burns
- Scrotal/genital burns
- Airway burns (if the unit has an ICU built in)
Examples of units are in these links:
Electrical Burns
Electricity contains a large amount of energy, and when passing through the body, it causes damage along its path and usually manifests itself as a burn at the entry and exit points.
Picture shows the entry wound of an electrical injury
Picture shows the exit wound on the leg.
There are a few modes of injury:
- Power points – The amount of damage caused by home/industrial mains depends on contact time, voltage and current.
- Lightning strikes, on the other hand, are rare but cause devastating injuries.
- A new phenomenon these days might be TASER burns in patients shot by police.
Assessment
A similar approach to assessment as thermal burns but beware of the lack or area affected. Electrical energy arcs into the body at small points but does tremendous damage along the route of the current all the way to the exit point. Thus a careful scan of the body and an ECG must be done to elicit damage. Muscle damage leads to breakdown called rhabdomyolysis and this, in turn, leads to renal failure and multi-organ failure if not treated promptly. Shoulder dislocations from being jolted from the electricity and head injuries are also common.
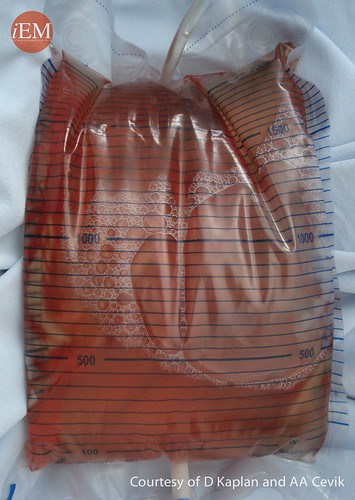
Picture shows urine of the patient who has rhabdomyolyis after electrical burn.
Lightning strikes have far more energy transmitted than household mains. Lichtenberg flowers are classically (but rarely) seen in lightning strike burns. Here lies a good write-up and picture of it.
Management
ED management includes:
- Analgesia – simple oral tablets to IV opioids depending on pain score
- Fluids – to prevent and treat renal failure
- Bicarbonate – in cases of rhabdomyolysis, alkalinization of the urine will help draw products of muscle break down out of the body.
- Treat other injured joints or organs sustained from the jolt when shocked (e.g., shoulder dislocations)
Escharotomy in a severely injured patient with high voltage electricity
Chemical/Radiation Burns
Picture shows chemical burn on the hand.
Picture shows chemical burn on the foot.
Like most toxic ingestions and exposures, the extent of injury depends on:
- Type of toxin
- Concentration of toxin
- Length of exposure to it
- Immediate decontamination and first aid
A good explanation of chemical burns from common household items can be found here.
Although radiation burns sound very ominous, they are handled similarly as all other burns. The myth that exposed patients can contaminate the whole hospital is unjustified and applies to only a specific scenario involving “dirty bombs.”
Most common radiation burns are actually from medical facilities such as cancer treatment or x-ray imaging centers as well as tanning booths and lamps. A good explanation of radiation damage and risks can be found in this pdf.
Assessment
A similar calculation for TBSA burned can be used as in thermal burns shown in the section above. However, the location of the burn and concentration of the agent have far more impact.
For example:
- Alkali burns of the cornea can result in permanent blindness
- Hydrofluoric acid burns can result in systemic fluorosis which is life-threatening
- Corrosive burns to the esophagus can cause permanent swallowing difficulties
Hence a thorough examination is more important than any lab or imaging test. Geiger counters can be used to detect contaminated patients exposed to radionuclides. This needs to be done by experts in the field.
Management
Probably the most important interventions to get right are the first aid processes:
- Removal of offending agent
- Irrigation with water to dilute and neutralize
- Transport to a medical facility
ED management includes;
- Analgesia – IV opioids most commonly as they are deep dermal burns
- More irrigation of the affected area if symptoms or pain persists
- Irrigation of the eyes is of utmost importance and the only way of removing the offending agent.
- Local anesthetic also helps during irrigation. A good video of this is shown below:
- Anti-tetanus toxoid
- Specific antidotes:
- Hydrofluoric acid – this acid is one of the most corrosive known and its systemic effects lower calcium to a life-threatening level. Hence calcium is essential not only for cardiac stability but also for analgesia. Calcium can be given in oral, topical gel and IV forms.
- Radionuclide poisoning – decontamination is once again dealt very comprehensively in this pdf.
- Referral to the burn unit
Inhalation injuries
Thermal inhalational injury
- Airways can become swollen due to inflammation. Prompt airway protection measures need to be initiated before the swelling becomes too severe (impairs breathing)
- Tracheobronchial edema / inflammation
- Acute Respiratory Distress Syndrome (ARDS) or acute lung injury
Smoke inhalation
- Particulate matter in smoke causes airway and bronchial inflammation which can lead to pulmonary edema, bronchospasm, and even ARDS. Signs of such injury include soot in the oropharynx, singed nasal hairs, hoarseness, stridor or confusion/agitation.
Chemical inhalational injury
When patients are thermally injured, the environment they were in can cause harm as well. Here are two of the most common inhalation injuries that patients trapped in burning environments receive.
- CO poisoning – This gas is a by-product of combustion. Symptoms can range from confusion to coma. The only way to detect it is a high degree of suspicion and via arterial blood gas. The treatment is 100% oxygen. In some cases with neurological symptoms and coma, hyperbaric oxygen therapy is recommended.
- CN poisoning – This gas is produced when furniture and other plastics are combusted (usually house fires). It is a pulmonary irritant and can cause tissue hypoxia which may lead to cardiac arrest. Treatment is decontamination, oxygen and specific antidotes (not in the scope of this section).
References and Further Reading
- Wikipedia page on skin – https://en.wikipedia.org/wiki/Skin
- Classification of burns. Phillip L Rice, Jr, MD, Dennis P Orgill, MD, PhD. UpToDate Oct. 2015
- The BEAM survival calculator for ICU, Alfred Hospital, Australia & ANZICS CORE – http://www.beamsurvival.com/
- Initial management of a major burn: II—assessment and resuscitation. BMJ. 2004 Jul 10; 329(7457): 101–103. – http://www.ncbi.nlm.nih.gov/pmc/articles/PMC449823/
- Victoria Burns Service, Alfred Hospital, Australia – http://www.vicburns.org.au/burns-assessment/total-body-surface-area/paediatric-burns-assessment.html
- Interview on Channel News Asia by Dr Rahul Goswami (author of this chapter). -https://youtu.be/3FSYbZMVPCs
- Burn Centre at the University of Washington – https://youtu.be/vKa4Aa1C0J8
- MDCalc. 2015 – http://www.mdcalc.com/parkland-formula-for-burns/#about-equation
- Victoria Burns Service, Alfred Hospital, Australia -http://www.vicburns.org.au/downloadable-evidence-summaries.html
- Kane Guthrie, Life in the Fast Lane EM blog. – http://lifeinthefastlane.com/minor-burns-in-the-emergency-department/
- ERJedi EM blog. – http://erjedi.com/2011/02/22/lightning-flowers/
- Mark P.Brady, Cambridge, MA USA. 60 Second EM blog. – http://www.60secondem.com/archives/1066
- Radiation Emergency Assistance Centre/Training Site. Oak Ridge Institute for Science and Education – https://orise.orau.gov/reacts/resources/radiation-accident-management.aspx
- Radiation Emergency Assistance Centre/Training Site. Oak Ridge Institute for Science and Education https://orise.orau.gov/files/reacts/medical-aspects-of-radiation-incidents.pdf
- Dr Alfred Sacchetti (YouTube channel) – https://youtu.be/-zhtmNHrRiU
- Prehospital Trauma and Life Support 8th Edition (National Association of Emergency Medical Technicians
- Prof Larry Mellick (YouTube channel) – https://youtu.be/6tclyWBPOak
- Emergency Medicine: A comprehensive study guide. Tintinalli 6th Edition, Section 15: page 1223