You have a new patient!
A 55-year-old male with alcoholic liver cirrhosis was brought to the emergency department by his wife, presenting with two episodes of haematemesis (containing fresh blood) and light-headedness. This is the first occurrence of such symptoms. Vital signs: Temperature: 36.8°C, Heart Rate: 115 bpm, SpO₂: 95%, BP: 88/65 mmHg. On examination, the patient appears pale, lethargic, and jaundiced, with abdominal distension noted.

What do you need to know?
Upper gastrointestinal (GI) bleeding is defined as bleeding occurring above the level of the ligament of Treitz. It is more common than lower GI bleeding [1]. Upper GI bleeding is a significant clinical condition that can lead to morbidity and mortality if not promptly diagnosed and managed. It encompasses bleeding from the esophagus, stomach, or duodenum, often presenting as hematemesis or melena. The importance of recognizing and treating upper GI bleeding lies in its potential to indicate serious underlying conditions. Early intervention is crucial, as the severity of bleeding can lead to hypovolemic shock, necessitating urgent medical care. Upper GI bleeding is a common emergency, with an estimated incidence of 50 to 150 cases per 100,000 individuals annually [2]. The prevalence varies based on demographic factors such as age, gender, and geographical location. The condition is more prevalent in older adults, particularly those over 60 years.
The most common cause is peptic ulcer disease, with duodenal ulcers being the most frequent. Other causes include varices, erosive esophagitis, duodenitis, Mallory-Weiss tear, gastrointestinal malignancies, and arterial and venous malformations (e.g., aorto-enteric fistula, Dieulafoy lesion) [1,3]. Causes of peptic ulcer disease include NSAID (Non-Steroidal Anti-inflammatory Drug) intake, Helicobacter pylori infection, and stress ulcers. In recent years, the incidence of upper gastrointestinal bleeding admissions due to peptic ulcer disease has decreased in the USA. This trend has been attributed to the use of triple therapy for Helicobacter pylori and the co-administration of proton pump inhibitors with NSAIDs [4].
Clinical manifestations include vomiting coffee ground material or fresh blood, and/or passing fresh blood in the stool or black, tarry stool (melena) [1].
Goals in the management of a patient with upper gastrointestinal bleeding include identifying the site and nature of the bleeding, stabilizing the patient, and controlling the source of the bleed [4].
Medical History
After performing a primary survey and stabilizing the patient, it is important to fine-tune your history, physical examination, and investigations to identify the source of bleeding and guide further management and disposition.
Upper GI bleeding commonly presents with haematemesis (coffee-ground or fresh blood), haematochezia, and/or melena [4]. Certain foods, such as beets, and medications like cefdinir, can cause red-colored stool, while bismuth and iron supplements may cause black-colored stool [4].
Associated Symptoms
- Peptic ulcer disease may be associated with epigastric pain (gastric ulcer) and dysphagia, gastroesophageal reflux disease (GERD), or odynophagia (esophageal ulcer).
- Haematemesis associated with retching may indicate a Mallory-Weiss tear.
- The presence of jaundice and ascites suggests variceal bleeding [4].
A prior history of GI bleeding should be assessed, as patients are more likely to bleed from the same lesion.
Key Past Medical History and Risk Factors
Peptic Ulcer Disease:
- Ulcers can occur in the esophagus, stomach, or duodenum, with duodenal ulcers being more common.
- However, gastric ulcers account for a higher incidence of bleeding.
- Known causes include Helicobacter pylori, NSAIDs, alcohol, and steroid use.
- Symptoms may include epigastric pain, nausea, vomiting, upper GI bleeding (painless haematemesis and melena), and signs of anaemia.
- Upper GI bleeding after NSAID use, stress, or a history of dyspepsia may indicate erosive gastritis [5,6].
Esophageal Varices:
- Caused by portal hypertension secondary to liver diseases such as cirrhosis.
- Symptoms include jaundice, spider angiomata, palmar erythema, hepatic encephalopathy (confusion), coagulopathy (petechiae/purpura), ascites, and variceal bleeding (painless haematemesis with large amounts of fresh blood) [6].
- Ask about chronic alcohol use, hepatitis, and hepatocellular carcinoma.
Mallory-Weiss Syndrome:
- Caused by forceful retching or vomiting, often after heavy alcohol intake.
- Leads to a tear in the esophagus or stomach, resulting in haematemesis (large amounts of fresh blood).
- This condition is usually self-limiting [6].
Malignancy:
- Gastric cancers may present with haematemesis, anaemia, and dyspepsia [6].
- Enquire about sudden weight loss, loss of appetite, and risk factors like prior Helicobacter pylori infection.
Angiodysplasia:
- Dieulafoy’s disease is a rare vascular malformation affecting young individuals.
- It involves small aneurysms in the stomach that rupture, leading to massive spontaneous haematemesis [6].
Aorto-enteric Fistula:
- A rare condition, usually occurring post-repair of an abdominal aortic aneurysm.
- Presents with profuse haematemesis and rectal bleeding [6].
Gastro-enteric Anastomosis:
- Ulcers may develop at the site of gastro-enteric anastomosis, presenting with upper GI bleeding [7].
Comorbid Illnesses
Enquire about conditions such as:
- Ischemic heart disease or pulmonary conditions (higher haemoglobin levels required).
- Coagulopathies (may necessitate additional therapies).
- Dementia or hepatic encephalopathy (risk of aspiration due to altered mental state).
- Heart failure or renal failure (risk of fluid overload during blood transfusion).
Medication History
Assess for [8]:
- NSAIDs (associated with peptic ulcers).
- Anticoagulants and antiplatelets.
- Chemotherapeutic agents.
- Iron supplements (black stool).
Symptoms of Severe Bleeding and Poor Prognosis [1,4,7,9]
- Light-headedness, confusion, syncope (cerebral hypoperfusion).
- Chest pain and palpitations (coronary hypoperfusion) .
Physical Examination
The severity of bleeding should be assessed based on clinical signs of shock rather than the color of the blood [4]. Upper GI bleeding typically presents with haematemesis (frank blood or coffee-ground emesis) and/or melena [4]. In cases of brisk upper GI bleeding, the patient may present as vitally unstable with haematochezia [4].
Vital Signs
Monitor for signs of hemodynamic instability, including:
- Tachycardia, tachypnea, and hypotension [1,7].
- Supine hypotension is associated with greater blood loss than orthostatic hypotension [1].
General Examination
- Confusion may indicate hemodynamic instability.
- Gynecomastia may be seen in patients with liver disease [10].
- Haematemesis strongly suggests an upper GI bleed [4].
ENT Examination
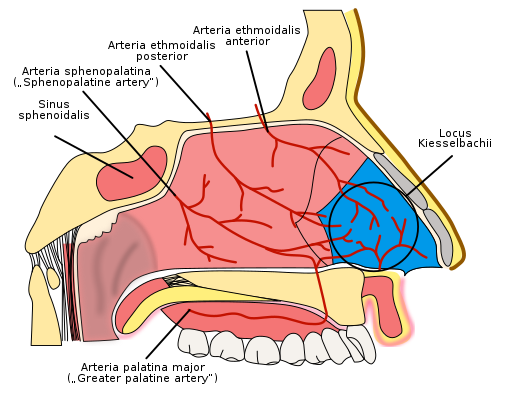
- Inspect the nose for epistaxis, which can present as haematemesis if the blood is swallowed [11].
Skin Examination
- Palmar erythema, spider angiomata, caput medusae, and jaundice are suggestive of liver disease [11].
Abdominal Examination
- Abdominal tenderness, guarding, rigidity, and rebound tenderness may indicate perforation.
- The presence of ascites suggests liver disease [4,7].
Rectal and Stool Examination
- A digital rectal examination and stool analysis can help identify the location of the bleed:
- Melena typically indicates an upper GI bleed.
- Haematochezia may suggest a lower GI bleed or a massive upper GI bleed [4].
Alternative Diagnoses
The differential diagnosis for gastrointestinal bleeding includes several conditions that may mimic an upper or lower GI bleed:
Epistaxis: Bleeding from the nose can present as haematemesis if the blood is swallowed. Careful examination of the nasal cavity is essential to rule this out.
Vaginal Bleeding: In some cases, vaginal bleeding can be mistaken for haematochezia. A thorough history and physical examination can help differentiate these sources.
Food-Induced Discoloration: Certain foods may alter the color of stool, leading to a false suspicion of GI bleeding. For example, beets can cause red-colored stools, which may mimic haematochezia.
Medication-Induced Changes: Some medications can also discolor stool:
- Cefdinir may produce red-colored stool.
- Iron supplements and bismuth-containing products can result in black stool, resembling melena [4].
Neonatal Swallowed Blood: In neonates, vomiting swallowed maternal blood during delivery or breastfeeding may be mistaken for upper GI bleeding [12].
Acing Diagnostic Testing
Bedside Tests
Several bedside tests can aid in the initial evaluation of upper GI bleeding:
- Point-of-care venous blood gas: Useful for detecting acidosis, electrolyte disturbances, and haemoglobin levels. Haemoglobin levels < 8 g/dL in previously healthy patients, or < 9 g/dL in patients with known coronary artery disease or anaemia-related complications, suggest the need for blood transfusion [4].
- Point-of-care PT (Prothrombin Time) and INR (International Normalized Ratio): Essential for patients taking medications like warfarin to determine the need for reversal agents.
- Bedside ultrasound: Helpful in identifying ascites, which may aid in diagnosing variceal bleeding.

Laboratory Tests
The following blood tests are useful when there is a clinical suspicion of upper GI bleeding [4,6,11,13]:
- Complete Blood Count (CBC): To assess haemoglobin and haematocrit levels.
- Blood Urea Nitrogen (BUN), Creatinine, and electrolytes: A BUN:Creatinine ratio > 35 is highly suggestive of upper GI bleeding (90%).
- Coagulation Screen: INR levels are important in patients on anticoagulant therapy (e.g., warfarin) to guide reversal strategies.
- Liver Function Tests: Elevated parameters are suggestive of liver disease and potential variceal bleeding.
- Type and Crossmatch: Crucial for patients who may require blood transfusion.
Imaging
Radiological imaging is rarely needed in hemodynamically unstable patients as it may delay resuscitation. In such cases, endoscopy should take precedence [4].
- Upright chest X-ray: Helpful in detecting free air under the diaphragm, which is suggestive of perforation.
- CT Angiography: Recommended for hemodynamically stable patients when identifying the bleeding etiology before endoscopy is crucial. It can detect slow bleeding (approximately 0.3 mL/min) and guide management decisions (endoscopy, surgery, or angiography). However, it is not suitable for unstable patients due to delays in management. In such cases, conventional angiography with embolization is preferred [4].
Endoscopy
Endoscopy is both diagnostic and therapeutic [14,15]:
- There is no evidence to support that emergent endoscopy is superior to routine endoscopy.
- Immediate gastroenterology consultation for emergent endoscopy is advised in patients with ongoing severe upper GI bleeding.
- Endoscopy is recommended within 24 hours for all admitted patients with UGIB after stabilizing hemodynamic parameters and addressing other medical issues.
- Patients with high-risk clinical features such as tachycardia, hypotension, haematemesis, or blood in nasogastric aspirate should undergo endoscopy within 12 hours, as this may improve clinical outcomes.
Additional Considerations
- A screening ECG is recommended in patients > 35 years of age with cardiac risk factors, as co-existing acute coronary syndrome may complicate GI bleeding [4].
- Nasogastric lavage is generally not recommended due to risks of perforation, pneumothorax, and aspiration [4].
- Erythromycin can be used as an alternative prokinetic to clear gastric contents before endoscopy [4,8].
Risk Stratification
To effectively manage gastrointestinal (GI) bleeding, patients must be categorized into high-risk and low-risk groups. High-risk patients require prompt intervention, whereas low-risk patients can be managed through outpatient treatment [4]. A combination of clinical, endoscopic, and laboratory features, along with risk scores, can aid in risk stratification. While risk scores may not always predict high-risk patients accurately, they are effective in identifying patients at very low risk of harm. When selecting patients for outpatient management, ensuring high sensitivity is essential to prevent the inadvertent discharge of high-risk individuals [16].
Risk Assessment Tools
Commonly used scoring systems for GI bleeding include:
- Glasgow-Blatchford Score (GBS)
- Rockall Score
- AIMS65 Score
The AIMS65 score assesses parameters such as:
- Albumin < 3 mg/dL
- International Normalized Ratio (INR) > 1.5
- Altered mental status
- Systolic blood pressure < 90 mmHg
- Age > 65 years
Studies show that the GBS is more effective at predicting a combined outcome of intervention or death [16].
Glasgow-Blatchford Score (GBS)
The Glasgow-Blatchford Score is particularly useful for predicting the need for intervention, hospital admission, blood transfusion, surgery, and mortality. A significant advantage of the GBS is that it can be calculated at the time of patient presentation, as it does not require endoscopic data (unlike the Rockall score).
The GBS includes the following parameters:
- Blood urea nitrogen (BUN)
- Haemoglobin levels
- Systolic blood pressure
- Pulse rate
- Symptoms such as melena, syncope, and a history of hepatic disease or cardiac failure.
The score ranges from 0 to 23, with a higher score indicating a greater risk of requiring endoscopic intervention [4].
Glasgow-Blatchford Risk Score
| Category | Score |
|---|---|
| BUN in mg/dL | |
| 18.2 to 22.4 | 2 |
| 22.5 to 28 | 3 |
| 28.1 to 70 | 4 |
| 70.1 or greater | 6 |
| Hemoglobin, men g/dL | |
| 12 to 13 | 1 |
| 10 to 11.9 | 3 |
| 9.9 or less | 6 |
| Hemoglobin, women g/dL | |
| 10 to 12 | 1 |
| 9.9 or less | 6 |
| Systolic Blood Pressure, mmHg | |
| 100-109 | 1 |
| 90-99 | 2 |
| <90 | 3 |
| Heartrate >100 peats per minute | 1 |
| Melena | 1 |
| Syncope | 2 |
| Hepatic Diseases | 2 |
| Heart failure | 2 |
Outpatient Management
Patients with a Glasgow-Blatchford Score of 0 are considered at low risk for rebleeding. According to international consensus guidelines, these patients may be safely discharged with early outpatient follow-up [8,17].
Management
Initial Stabilization
Airway and Breathing:
Patients with massive upper GI bleeding presenting with uncontrollable haematemesis, respiratory distress, or severe shock require immediate airway protection and intubation. It is essential to improve hemodynamic status before administering induction and paralytic drugs for intubation and initiating positive pressure ventilation, as this can mitigate a sharp decrease in cardiac output. However, intubation is associated with poor outcomes and should only be performed when absolutely necessary [4].
Circulation:
Massive GI haemorrhage is characterized by ongoing active bleeding (haematemesis or haematochezia), signs of hemodynamic compromise (e.g., tachycardia, hypotension, altered mental status), or a shock index ≥ 0.9 [4].
Immediate volume resuscitation is critical and includes:
- Placement of two large-bore IV catheters.
- Infusion of balanced isotonic crystalloids (e.g., 2 liters of normal saline or Plasmalyte over 30 minutes).
- Transfusion of uncrossmatched blood, if required [4].
Transfusion Strategies
For stable patients, a restrictive transfusion strategy is recommended. While the ideal haemoglobin target is not universally defined:
- In stable patients without known coronary artery disease (CAD), maintain haemoglobin ≥ 8 g/dL.
- For patients with known CAD, a higher target of ~9 g/dL is appropriate to reduce the risk of anaemia-related complications [4].
In patients requiring massive transfusion (more than 4 units of PRBCs), a balanced transfusion ratio of 1:1:1 (PRBC:Platelets:Fresh Frozen Plasma) is advised. Cryoprecipitate should be administered if fibrinogen levels remain < 1.5 g/L [18]. A platelet count > 50,000 platelets/μL should be maintained [4].
Coagulation Management
- Vitamin K antagonists (e.g., warfarin) should be stopped and reversed to achieve a target INR of 1.5–2.5. Treatment options include Fresh Frozen Plasma (FFP) and Prothrombin Complex Concentrate (PCC). Vitamin K is an appropriate choice for hemodynamically stable GI bleeding.
- Direct oral anticoagulant reversal:
- Idarucizumab for dabigatran reversal.
- PCC or coagulation factor Xa (recombinant/inactivated-zhzo) for factor Xa inhibitors.
- For heparin reversal, protamine sulfate may be used.
Before administering reversal agents, the risks of reversing anticoagulant therapy must be carefully weighed against the risk of thromboembolism [19].
PCC is preferred over FFP for rapid coagulopathy correction, especially in patients at risk of fluid overload, as it requires lower volume administration [4]. Over-transfusion or empiric correction of PT/INR with FFP or PCC in portal hypertension may worsen portal hypertension and exacerbate bleeding [4].
Medications
Proton Pump Inhibitors (PPIs)
PPIs are the mainstay in the management of acute GI bleeding. They work by inhibiting the hydrogen potassium ATPase pump, thereby reducing gastric acid secretion [20]. Studies have shown that PPIs reduce the risk of re-bleeding, the need for surgery, and mortality in patients with bleeding ulcers [4].
Both intermittent PPI therapy and continuous infusion are equally effective in reducing bleeding [8]. Available IV formulations include esomeprazole and pantoprazole. The recommended dose is:
- Pantoprazole or esomeprazole: 80 mg IV as a single initial dose, followed by either:
- Continuous infusion at 8 mg/hr, or
- 40 mg IV BID [8].
If IV formulations are unavailable, oral alternatives such as 40 mg of esomeprazole twice daily may be used [8].
PPIs are classified as Category B in pregnancy, except for omeprazole, which is Category C [21]. Caution should be exercised due to the risk of Clostridium difficile infection, Steven Johnson syndrome, kidney and liver impairment, and pancreatitis [20]. Omeprazole is particularly associated with the risk of acute interstitial nephritis [22].
Somatostatin Analogues
Somatostatin and its synthetic analogue, octreotide, are predominantly used in variceal bleeding. These agents reduce the risk of bleeding, need for transfusion, and portal hypertension. Indications include acute GI bleeding in patients with variceal bleeding, abnormal liver function tests, liver disease, or alcoholism [4].
The dosing regimen for octreotide is:
- Adults: 50 mcg IV bolus, followed by 25–50 mcg/hr continuous infusion [23,24].
- Paediatrics: 1 mcg/kg IV bolus (maximum: 100 mcg), followed by 1 mcg/kg/hr infusion [23,24].
Octreotide crosses the placenta and is expressed in breast milk. Common adverse effects include arrhythmias, pancreatitis, abnormal glucose regulation, and low platelet count [23]. It also crosses the blood-brain barrier [23].
Terlipressin
Terlipressin is a synthetic vasopressin receptor agonist that causes splanchnic vasoconstriction, thereby reducing portal hypertension. It is primarily indicated for variceal bleeding [25].
The recommended dose is 2 mg IV every 6 hours [26]. Terlipressin may cause teratogenic effects (limited data available) [27] and can result in painful hands and feet due to peripheral vasoconstriction [26]. While studies suggest that terlipressin, somatostatin, and octreotide have similar efficacy, data regarding their use in paediatric patients remains limited [24,28].
Prokinetic Agents (Erythromycin and Metoclopramide)
Prokinetic agents are used to improve visualization during endoscopy by clearing gastric contents.
Erythromycin:
- Adult dose: 3 mg/kg IV, administered over 20–30 minutes, 20–90 minutes before endoscopy [29].
- Classified as Category B in pregnancy and is safe for breastfeeding mothers [29].
- Adverse effects include QT prolongation, pseudomembranous colitis, seizures, and hypertrophic pyloric stenosis [4,29].
Metoclopramide:
- Adult dose: 10 mg IV.
- Paediatric dose: 0.1–0.2 mg/kg IV [30].
- Classified as Category B in pregnancy [30].
- Caution is advised in patients with a history of extrapyramidal symptoms due to its association with extrapyramidal side effects [30].
Tranexamic Acid
Tranexamic acid is an antifibrinolytic agent. However, according to the HALT-IT Trial, it has not been shown to reduce mortality associated with gastrointestinal bleeding. As a result, its routine use in GI bleeding is not recommended [31].
Antibiotic Prophylaxis
Antibiotic prophylaxis is recommended for patients with cirrhosis or suspected cirrhotic liver disease to reduce the risk of infection and mortality [4].
The recommended antibiotics include:
Fluoroquinolones (e.g., ciprofloxacin 400 mg IV)
Third-generation cephalosporins (e.g., ceftriaxone 1–2 g IV) [4].
Ceftriaxone: Classified as Category B in pregnancy but contraindicated in hyperbilirubinemic neonates due to the risk of kernicterus and those receiving IV calcium-containing solutions due to ceftriaxone–calcium precipitation [32].
Ciprofloxacin: Classified as Category C in pregnancy. Adverse effects include Clostridium difficile infection, dysglycemia, tendon rupture, neurotoxicity, QT prolongation, hepatotoxicity, and Stevens-Johnson syndrome/toxic epidermal necrolysis [33].
Procedures
Balloon tamponade [4,6,34], using devices such as the Sengstaken-Blakemore tube, Minnesota tube, or Linton-Nachlas tube, can serve as a temporizing measure for suspected life-threatening variceal bleeding when endoscopy is not immediately available. These devices must be stored in refrigerators to maintain readiness.
Before the procedure, patients must be intubated to reduce the risk of aspiration. The device is inserted through the mouth, passed via the esophagus into the stomach. The tube consists of two balloons—a gastric balloon and an esophageal balloon:
- The gastric balloon of the Sengstaken-Blakemore tube can be inflated with 250–300 cc of air, while the Minnesota tube can accommodate up to 450–500 cc to secure the tube in place.
- The esophageal balloon can be inflated to a pressure of 20–40 mmHg, with a strict upper limit of 45 mmHg to avoid injury. Pressure should be carefully monitored using a manometer.
Balloon tamponade is a temporary measure, and definitive management, such as endoscopic therapy, should be arranged as soon as possible. The procedure is associated with significant risks, including ulceration, esophageal rupture, and aspiration [4].
Special Patient Groups
Paediatrics
The causes of upper GI bleeding in the pediatric population are generally similar to those seen in adults [12,15,35]. However, there are additional causes specific to neonates and infants that require consideration. In neonates, vitamin K deficiency, also referred to as the haemorrhagic disease of the newborn, is an important cause. Other causes include congenital vascular anomalies, such as telangiectasia, and coagulopathy, which may result from infections, liver disease, or coagulation factor deficiencies. Milk protein intolerance is also a recognized cause of upper GI bleeding in this age group. During the neonatal period and the first few months of life, it is crucial to differentiate swallowed maternal blood from true upper GI bleeding. The Apt-Downey test is a reliable diagnostic tool used to confirm the presence of fetal blood and rule out swallowed maternal blood as the source.
The management of upper GI bleeding in children largely follows the same principles as in adults, with necessary adaptations for the pediatric population. Intravenous proton pump inhibitors (IV PPIs) are effective and can be administered to reduce gastric acid secretion, thereby promoting hemostasis. In cases of suspected variceal bleeding, somatostatin analogues can be given to reduce portal hypertension and minimize bleeding risk. When severe acute bleeding is ongoing, endoscopy plays a key role in diagnosis and intervention. It is recommended that endoscopy be performed within 24 to 48 hours of presentation. However, it is critical to ensure that the patient is as hemodynamically stable as possible before proceeding with the procedure to minimize complications.
In cases where endoscopy cannot control the bleeding or fails to identify the source, further interventions may be necessary. Angiography with embolization is a useful modality in such instances, as it can help detect and address underlying vascular abnormalities contributing to the bleeding. This approach is particularly helpful when other methods have proven unsuccessful.
Overall, a multidisciplinary approach that includes appropriate stabilization, pharmacologic therapy, and procedural intervention is essential to effectively manage upper GI bleeding in the pediatric population [12,15,35].
Geriatrics
Upper GI bleeding in elderly patients presents unique challenges due to the high-risk nature of this population and the limitations of existing risk assessment tools. Studies indicate that traditional pre-endoscopic risk scores, such as the Glasgow-Blatchford and AIMS65, often fail to accurately predict outcomes like mortality and hospital stay length in geriatric patients, particularly those aged 82 and older, suggesting a need for age-adjusted scoring systems [36]. Despite these challenges, emergency oesophagogastroduodenoscopy is generally safe for elderly patients, with a high survival rate at 90 days post-procedure, although a significant proportion of OGDs yield normal findings, highlighting the importance of careful patient selection [37]. The management of Upper GI bleeding in the elderly is further complicated by recurrent bleeding, as seen in cases involving peptic ulcer disease, which necessitate a multidisciplinary approach and close monitoring to improve outcomes [38]. Recent efforts to develop novel risk scores tailored for the elderly have shown promise, with a new score incorporating factors like comorbidity index and blood pressure demonstrating good discriminative performance for identifying patients suitable for outpatient management [39].
Pregnant Patients
The causes of upper GI bleeding in pregnant women are similar to those in the general population, including conditions such as esophageal ulcers, gastroesophageal reflux disease, and portal vein thrombosis leading to esophageal varices [40]. Haematemesis, or the vomiting of blood, is a common manifestation of upper GI bleeding and can present as bright red or coffee-ground emesis, indicating bleeding from the upper gastrointestinal tract [1, 40]. In rare cases, UGIB in pregnancy can be caused by gastrointestinal stromal tumors (GISTs), as illustrated by a case where a pregnant woman presented with coffee-ground vomiting and was diagnosed with a bleeding GIST at the stomach cardia [41]. Endoscopy is a critical diagnostic and therapeutic tool for upper GI bleeding, but its use in pregnant women is generally reserved for severe or persistent cases due to potential risks to the mother and fetus [42]. Despite the need for endoscopic evaluation in over 12,000 pregnant women annually in the U.S., research on the safety and outcomes of such procedures remains limited [43]. Therefore, careful consideration of the risks and benefits is essential when managing upper GI bleeding in pregnant patients.
When To Admit This Patient
Admission is required for elderly patients over the age of 60 years, those who require blood transfusions, and patients with a Glasgow-Blatchford Score (GBS) greater than 0 [4,8]. Patients with high-risk bleeding sources should be admitted to a monitored setting or an intensive care unit (ICU) to allow close monitoring for signs of rebleeding and other potential complications.
The decision to discharge a patient following endoscopy depends on the identification of the bleeding source and the associated risk of rebleeding. Patients can be considered for discharge if they meet all of the following criteria: a GBS of 0, blood urea nitrogen (BUN) less than 18 mg/dL, haemoglobin >13 g/dL in men and >12 g/dL in women, heart rate less than 100 beats per minute, systolic blood pressure greater than 110 mmHg, no evidence of melena or syncope since the initial presentation, absence of heart failure or liver failure, and prompt access to outpatient follow-up care.
However, it is important to note that this recommendation is based on low-quality evidence, and clinical judgment should play a significant role in the final decision to discharge a patient. Clinicians should carefully assess each patient’s overall condition, risk of rebleeding, and ability to follow up in an outpatient setting to ensure safe discharge planning [15].
Revisiting Your Patient
In managing this patient, the immediate priority is to assess airway, breathing, and circulation and provide stabilization. Given the patient’s vital instability, they should be promptly transferred to the resuscitation bay for further management.

Airway and Breathing: The patient’s airway is currently patent, and they are communicating comfortably, with no signs of obstruction such as pooling of blood or secretions. There have been no further episodes of haematemesis, and the patient is maintaining adequate oxygen saturation on room air. Chest auscultation is clear. At this time, the patient does not require airway adjuncts or intubation, but close observation is essential to detect any deterioration.
Circulation: The patient is hypotensive, indicating the need for immediate intervention. Two large-bore IV cannulas should be inserted to initiate intravenous fluid resuscitation. Crossmatched and uncrossmatched blood should be arranged as a precaution. A point-of-care venous blood gas test must be performed to quickly evaluate acidosis, haemoglobin levels, and other critical parameters. Care should be taken to avoid fluid overload, especially in patients with underlying liver disease.
Further History and Review of Systems: On further evaluation, the patient denies haematochezia, haemoptysis, epistaxis, melena, chest pain, palpitations, syncope, loss of consciousness, or confusion.
Past Medical and Surgical History and Risk Factors: The patient has a history of alcoholic liver disease and is a smoker. There is no history of chronic NSAID use, Helicobacter pylori infection, recent forceful retching, or ingestion of foods or medications that might cause red-colored secretions. There are no known coagulopathies, recent anticoagulant use, vascular abnormalities, weight loss, or loss of appetite. Additionally, the patient has no history of prior surgery.
Examination: Clinical signs of hemodynamic instability, such as hypotension, suggest hypovolemic shock, requiring prompt management with IV fluids and blood transfusion. Examination findings of jaundice, abdominal distension with shifting dullness, and caput medusae are consistent with alcoholic liver disease and indicate probable variceal bleeding. There is no abdominal tenderness, guarding, rigidity, or rebound tenderness to suggest another abdominal pathology.
Laboratory Investigations: Laboratory tests sent include a complete blood count, urea, electrolytes, creatinine, coagulation screen, liver function tests, and type and crossmatch for transfusion. The point-of-care venous blood gas reveals acidosis, haemoglobin <8 g/dL, negative base excess, and elevated lactate, indicating ongoing active bleeding. These findings necessitate urgent gastroenterology consultation for endoscopic intervention and the arrangement of blood transfusion. In addition, the patient must be monitored for liver disease-induced coagulopathy, and a haematology consultation is warranted.
Diagnostic Test: The patient’s Glasgow-Blatchford Score is greater than 0, further confirming the need for urgent endoscopy to identify and control the source of bleeding, which is most likely esophageal varices. Simultaneously, resuscitation measures must continue.
Medications: Given the patient’s history of alcoholic liver disease and suspected variceal bleeding, appropriate pharmacological management should include vasoactive agents such as somatostatin, octreotide, or terlipressin to reduce portal pressure. Empirical antibiotics (fluoroquinolones or third-generation cephalosporins) should be administered to reduce the risk of infection. Additionally, proton pump inhibitors (PPIs) should be started as part of the management protocol.
Disposition: This patient requires urgent gastrointestinal consultation for endoscopy to achieve source control of the bleeding. Admission is necessary to allow for close monitoring of potential complications, including rebleeding and complications of alcoholic liver cirrhosis, such as hepatic encephalopathy and renal failure.
Authors

Resshme Kannan Sudha
Resshme Kannan Sudha graduated from RAK Medical and Health Sciences University and is currently an Emergency Medicine Graduate Resident at STMC Hospital, Al Ain. She is a keen follower of FOAMed projects and an enthusiastic educator. Her special interests include critical care, POCUS, global health, toxicology and wilderness medicine.

Thiagarajan Jaiganesh
STMC Hospital, Al Ain
Listen to the chapter
References
- Antunes C, Copelin II EL. Upper gastrointestinal bleeding – StatPearls – NCBI Bookshelf. Upper Gastrointestinal Bleeding. Published July 18, 2022. Accessed March 17, 2023. https://www.ncbi.nlm.nih.gov/books/NBK470300/
- Southwood KE. Upper gastrointestinal bleeding. Gastroenterology Nursing. Published ahead of print. 2023. doi:10.1097/SGA.0000000000000743
- Carrol M, Mudan G, Bentley S. Gastrointestinal bleeding. International Emergency Medicine Education Project. Published February 18, 2019. Accessed March 17, 2023. https://iem-student.org/gi-bleeding/
- DeGeorge LM, Nable JV. Gastrointestinal bleeding. In: Rosen’s Emergency Medicine: Concepts and Clinical Practice. 10th ed. Philadelphia, PA: Elsevier; 2023:240-244.
- Donaldson R, Swartz J, Ong M, et al. Peptic ulcer disease – WikEM. WikEM. Published December 7, 2022. Accessed April 11, 2023. https://www.wikem.org/wiki/Peptic_ulcer_disease
- Leach T. Upper GI bleed. Almostadoctor. Published December 5, 2020. Accessed April 8, 2023. https://almostadoctor.co.uk/encyclopedia/upper-gi-bleed
- Pace R. Upper GI bleeding. Core EM. Published January 24, 2018. Accessed March 20, 2023. https://coreem.net/core/upper-gi-bleeding/
- Undifferentiated upper gastrointestinal bleeding – WikEM. WikEM. Accessed March 23, 2023. https://www.wikem.org/wiki/Undifferentiated_upper_gastrointestinal_bleeding
- Kaur G. Upper gastrointestinal bleeding: Evaluation, management, and disposition. emDOCs.net – Emergency Medicine Education. Published June 7, 2021. Accessed April 11, 2023. https://www.emdocs.net/upper-gastrointestinal-bleeding-evaluation-management-and-disposition/
- Chen ZJ, Freeman ML. Management of upper gastrointestinal bleeding emergencies: evidence-based medicine and practical considerations. World J Emerg Med. 2011;2(1):5-12. doi:10.5847/wjem.j.1920-8642.2011.01.001
- (Sokolosky MC. Gastrointestinal bleeding. In: Tintinalli’s Emergency Medicine Manual. New York, NY: McGraw-Hill Education; 2018:237-238.
- Donaldson R, Swartz J, Claire, et al. Gastrointestinal bleeding (peds) – WikEM. WikEM. Updated March 29, 2022. Accessed April 10, 2023. https://www.wikem.org/wiki/Gastrointestinal_bleeding_(peds)
- Wilkins T, Wheeler B, Carpenter M. Upper gastrointestinal bleeding in adults: Evaluation and management. American Family Physician. Published March 1, 2020. Accessed March 20, 2023. https://www.aafp.org/pubs/afp/issues/2020/0301/p294.html
- Laine L, Barkun AN, Saltzman JR, Martel M, Leontiadis GI. ACG clinical guideline: Upper gastrointestinal and ulcer bleeding. Am J Gastroenterol. 2021;116(5):899-917. doi:10.14309/ajg.0000000000001245
- Woodfield A, Donaldson R, Reynolds C, Young N. Upper GI bleeding guidelines. WikEM. Published March 12, 2022. Accessed March 20, 2023. https://www.wikem.org/wiki/Upper_GI_bleeding_guidelines
- Stanley AJ, Laine L. Management of acute upper gastrointestinal bleeding. BMJ. 2019;364:l536. Published March 25, 2019. Accessed February 15, 2023. https://www.bmj.com/content/364/bmj.l536
- Barkun AN, Almadi M, Kuipers EJ, et al. Management of nonvariceal upper gastrointestinal bleeding: Guideline recommendations from the International Consensus Group. Ann Intern Med. 2019;171(11):805. doi:10.7326/m19-1795
- Farkas J. GI bleeding. EMCrit Project. Published September 18, 2021. Accessed April 11, 2023. https://emcrit.org/ibcc/gib/
- Gnanapandithan K, Muniraj T. Management of antithrombotics around gastrointestinal procedures. PubMed. Published 2023. Accessed April 11, 2023. https://www.ncbi.nlm.nih.gov/books/NBK553210/
- Carmen Fookes B. List of proton pump inhibitors + uses, side effects. Drugs.com. Accessed April 11, 2023. https://www.drugs.com/drug-class/proton-pump-inhibitors.html
- Richter JE. Gastroesophageal reflux disease during pregnancy. Gastroenterol Clin North Am. 2003;32(1):235-261. doi:10.1016/s0889-8553(02)00065-1
- Reynolds C, Cunningham R, Ostermayer D, Donaldson R, Young N. Omeprazole. WikEM. Updated March 5, 2021. Accessed April 11, 2023. https://wikem.org/wiki/Omeprazole
- Ostermayer D, Murray B, Lee E, Donaldson R, Cunningham R. Octreotide. WikEM. Published February 10, 2021. Accessed March 20, 2023. https://wikem.org/wiki/Octreotide
- Sandostatin, Sandostatin LAR (octreotide) dosing, indications, interactions, adverse effects, and more. Medscape. Accessed April 11, 2023. https://reference.medscape.com/drug/sandostatin-lar-octreotide-342836
- Nickson C. Terlipressin. Life in the Fast Lane. Published January 4, 2019. Accessed April 11, 2023. https://litfl.com/terlipressin/
- Tripathi D, Stanley AJ, Hayes PC, et al. UK guidelines on the management of variceal haemorrhage in cirrhotic patients. Gut. 2015;64(11):1691-1692. doi:10.1136/gutjnl-2015-309262
- Terlivaz. Medscape. Published July 15, 2024. Accessed December 7, 2024. https://reference.medscape.com/drug/terlivaz-terlipressin-4000107#6
- Seo YS, Park SY, Kim MY, et al. Lack of difference among terlipressin, somatostatin, and octreotide in the control of acute gastroesophageal variceal hemorrhage. Hepatology. 2014;60(3):962. doi:10.1002/hep.27006
- Donaldson R, Claire, Lee E, Ostermayer D, Holtz M. Erythromycin. WikEM. Published September 22, 2019. Accessed March 20, 2023. https://www.wikem.org/wiki/Erythromycin
- Fernando T, Donaldson R, Grove G, et al. Metoclopramide. WikEM. Updated March 7, 2021. Accessed April 11, 2023. https://www.wikem.org/wiki/Metoclopramide
- Roberts I, Shakur-Still H, Afolabi A, et al. Effects of a high-dose 24-h infusion of tranexamic acid on death and thromboembolic events in patients with acute gastrointestinal bleeding (HALT-IT): an international randomised, double-blind, placebo-controlled trial. Lancet. 2020;395(10241):1927-1936. doi:10.1016/s0140-6736(20)30848-5
- Donaldson R, Shah M, Ostermayer D, Young N, Claire. Ceftriaxone. WikEM. Updated September 19, 2019. Accessed April 10, 2023. https://www.wikem.org/wiki/Ceftriaxone
- Donaldson R, Gausepohl A, Janeway H, et al. Ciprofloxacin. WikEM. Updated October 17, 2021. Accessed April 11, 2023. https://wikem.org/wiki/Ciprofloxacin
- Balloon tamponade for massive GI bleeding – WikEM. WikEM. Accessed March 23, 2023. https://www.wikem.org/wiki/Balloon_tamponade_for_massive_GI_bleeding
- Lirio RA. Management of upper gastrointestinal bleeding in children. Gastrointest Endosc Clin N Am. 2016;26(1):63-73. doi:10.1016/j.giec.2015.09.003
- Di Gioia G, Sangineto M, Paglia A, et al. Limits of pre-endoscopic scoring systems in geriatric patients with upper gastrointestinal bleeding. Sci Rep. 2024;14(1). doi:10.1038/s41598-024-70577-2.
- McWhirter A, Mahmood S, Mensah E, Nour H, Olabintan O, Mrevlje Z. Evaluating the safety and outcomes of oesophagogastroduodenoscopy in elderly patients presenting with acute upper gastrointestinal bleeding. Cureus. 2023. doi:10.7759/cureus.47116.
- Ahmad H, Khan U, Jannat HE. Recurrent gastrointestinal bleeding in an elderly patient with peptic ulcer disease: successful management through multidisciplinary intervention and close monitoring. Cureus. 2023. doi:10.7759/cureus.41468.
- Li Y, Lu Q, Song M, Wu K, Ou XL. Novel risk score for acute upper gastrointestinal bleeding in elderly patients: a single-centre retrospective study. BMJ Open. 2023;13(6):e072602. doi:10.1136/bmjopen-2023-072602.
- Shahid S, Chandra N. Haematemesis in pregnancy. In: Gastrointestinal Emergencies in Pregnancy. CRC Press; 2015:149-153. doi:10.1201/B18646-36.
- Parampalli U, Crossland C, Longley J, Morrison I, Sayegh M. A rare case of gastrointestinal stromal tumour in pregnancy presenting with upper gastrointestinal bleeding. J Gastrointest Cancer. 2012;43(1):80-83. doi:10.1007/s12029-011-9360-3.
- Bjorkman DJ. Is endoscopy safe for pregnant women with upper gastrointestinal bleeding. NEJM J Watch. 2011. doi:10.1056/JG201101070000004.
- Rabiee A, Moshiree B. Upper and lower endoscopy for gastrointestinal (GI) bleeding in pregnancy. In: Gastrointestinal Bleeding. Springer; 2019:155-164. doi:10.1007/978-3-319-90752-9_12.
Reviewed and Edited By

Arif Alper Cevik, MD, FEMAT, FIFEM
Prof Cevik is an Emergency Medicine academician at United Arab Emirates University, interested in international emergency medicine, emergency medicine education, medical education, point of care ultrasound and trauma. He is the founder and director of the International Emergency Medicine Education Project – iem-student.org, chair of the International Federation for Emergency Medicine (IFEM) core curriculum and education committee and board member of the Asian Society for Emergency Medicine and Emirati Board of Emergency Medicine.
Sharing is caring
- Share on X (Opens in new window) X
- Share on Reddit (Opens in new window) Reddit
- Share on LinkedIn (Opens in new window) LinkedIn
- Share on Facebook (Opens in new window) Facebook
- Share on Tumblr (Opens in new window) Tumblr
- Share on Pinterest (Opens in new window) Pinterest
- Share on WhatsApp (Opens in new window) WhatsApp
- Email a link to a friend (Opens in new window) Email
- Print (Opens in new window) Print