Mental health conditions are the leading cause of disability worldwide, accounting for an estimated 175.3 million years lost to disability (Figure 1). Inequalities in access to or quality of mental health care globally are directly related to social, structural, and economic determinants. Increasingly, research suggests that these socioeconomic inequalities lead to health issues not just for disadvantaged populations but for all those involved in unjust or unequal societies. In addition, most of our information on global access to mental health care is limited to formal psychiatric care, which discounts other forms of local or indigenous healing practices.

Disasters have countless impacts on communities and can cause stress due to feelings of powerlessness, loss of community life and culture, and destruction and physical displacement. An estimated 1 in 3 highly exposed trauma survivors may experience post-traumatic stress disorder (PTSD), and 1 in 4 may experience major depression. Psychological distress, which does not meet the criteria for another formal psychiatric diagnosis, is nearly universal after exposure to a disaster and deserves significant attention as well.
It is also crucial to ensure that mental health responses after disasters are conscious of unique local contexts. Previously, priorities in disaster responses have primarily been defined by mental health professionals mostly by nations of the Global North, which gives insufficient attention to locally-defined priorities. These established programs focus mainly on major neuropsychiatric disorders as defined by Western professionals and assume that the features, courses, and outcomes will mirror those seen in the cultures where they were initially developed. Existing programs and literature also tend to focus on PTSD, with other forms and manifestations of psychological distress falling through the cracks. This focus on applying formal diagnosis and treatment assumes that they are generalizable across cultures and may marginalize indigenous forms of healing that could be vital to the community.
Key Priorities
With these concerns in mind, we want to highlight some key priorities in creating a culturally sensitive mental health care program in the post-disaster setting. First, we need to remember that systemic factors such as structural violence and poverty are important determinants of mental health outcomes (Figure 2). Thus it is imperative to first support efforts addressing basic socioeconomic needs and promote physical safety of the population. In addition, mental health programming may be carried out in tandem with medical colleagues addressing other problems to increase coverage and decrease the need for additional infrastructure.
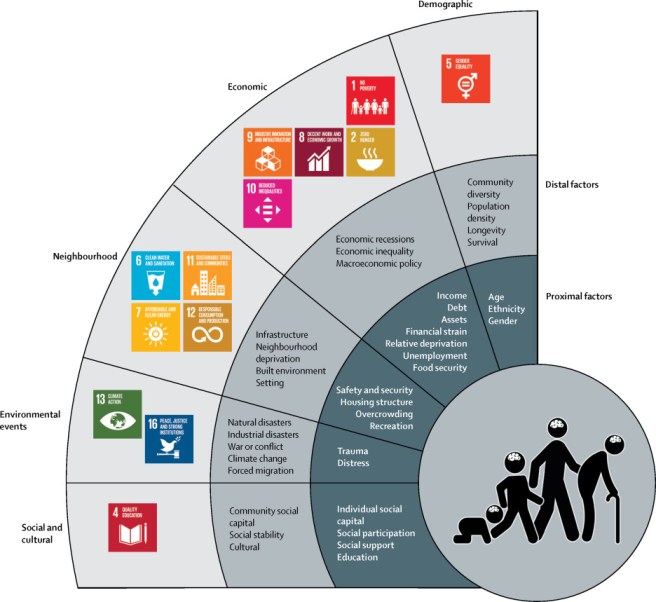
Figure 2: Proximal and distal factors of the social determinants of mental health with sustainable development goals mapped onto the different domains.
In assessing the community’s mental health needs, there should be an effort to learn and adapt to the local context, as an individual’s response to suffering is likely influenced by the religious, spiritual, and moral context of the local community. In addition, classification systems used in mental health evaluation (i.e., DSM-5) should be modified to integrate the knowledge of culturally specific idioms of stress, taking into account also differences related to class, gender, age, sexuality, minority/majority position. Lastly, special attention must be given to those with existing psychopathology as these individuals are at risk of having worse outcomes in response to disasters.
Proposed Solution
Guided by these principles, we proposed examples of programming components that partner with the local community and integrate an understanding of local resources and traditions of healing.
- Work with psychologists, community health workers, and local religious leaders to facilitate memorial services in response to possible losses in the community.
- Promote education on when and where to seek service, especially in social settings that communities frequently gather.
- Develop programs that go beyond the toolkit of professionals and mobilize indigenous resources and family-specific social activities to encourage people to also rely on support from immediate social networks.
- Partner with specialists to support task-shifting to local non-specialist providers.
- Establish screening protocols for aid workers and staff working in disaster settings as these individuals are also at risk for mental health issues.
We want to have a continuous evaluation of the program in four outcomes areas, each with different indicators:
- Relevance (indicated by population need and cultural and contextual fit)
- Effectiveness (indicated by mental health outcome)
- Quality (indicated by adherence, competence, and attendance)
- Feasibility (indicated by coverage and cost)
While some of the indicators, such as coverage, helps to define operational characteristics of the program, other factors, such as cultural and contextual need, support the program by engaging with local stakeholders. Information regarding these indicators can be obtained using various methods, including community surveys, national health system records, cohort studies, and observational studies.
Though the world’s mental health burden is experienced heavily in low and middle-income countries (LMICs), often only a tiny portion of the annual operating health budgets in these countries will go toward addressing mental health issues. For example, the Emerald (Emerging mental health systems in LMICs) study, which was a multinational study conducted to assess the infrastructural and policy needs for expanding mental health services in Ethiopia, India, Nepal, Nigeria, South Africa, and Uganda, revealed that in some LMICs, there is less than $0.25 per person per year available for mental health budgeting. In addition to limited resources and finances, mental health programs face other challenges related to sustainability, such as poorly trained staff and a lack of understanding about service delivery processes and quality improvement. High turnover of senior-level policymakers can prevent longitudinal advocacy and agenda-setting, and low community participation can also be a barrier.
While the exact cost for our program is difficult to predict given system collapse and displacement of populations in the post-disaster setting, here we provide an estimation of a possible budget using the operating budget of the NGO Médecins Sans Frontières (MSF) in 2020 as a starting point.
- MSF Operating Budget 2020 = €550,000,000 Euros, with 80% spent on programming spending (€440,000,000)
- €440,000,000 spent across 10 countries = €44,000,000/country in 2020
- *Presuming 2% for mental health budget allocation = €880,000 for mental health budget/country/year
- ~350,000 Mental Health Consultations across 10 countries
- ~35,000 Mental Health consultations annually per nation engaged
- €880,000 / 35,000 consultations = €25/consultation (used for medications, counseling, etc)
Even assuming just 2% of the operations budget is allocated to mental health programming, it can be estimated that major NGOs may be able to make a more significant fiscal investment in mental health than what public services can currently offer in LMICs. In the emergent setting, the surge of financial resources from these agencies towards affected groups presents new opportunities and motivation for development. Additionally, the destruction or collapse of health systems amidst destabilization may provide opportunities to build more equitable and person-centered care systems. Furthermore, media attention can stir public interest and political willpower to dedicate more resources to mental health treatment systems.
Historically, international health actors have not prioritized the transition of care from transient emergent systems to nascent local infrastructure. Thus two types of investment are needed to ensure a smooth transition and subsequent strengthening of the local health system. Initially, startup investment from aid organizations is needed to maintain operating budgets amidst transitions. Then continuous funding for long-term service delivery from health departments or public agencies is required to promote infrastructure longevity and tackle some of the previously mentioned system-level challenges impeding sustainability of programming.
Summary
In summary, our current understanding of and approach to global mental health focus on priorities does not pay sufficient attention to local priorities and marginalizes indigenous healing techniques. Guided by an understanding of the social determinants of mental health, at-risk populations in disaster settings, and the crucial importance of adapting to local contexts, we proposed several priorities in infrastructure support, assessment, and intervention when establishing culturally sensitive mental health care programs. Outcomes of the program will then be evaluated in its relevance, effectiveness, quality, and feasibility and used to modify the program in response to changing needs in the post-disaster setting. While the increase in support from NGOs during times of disaster will likely result in increased resources available for mental health programming, transition, and down-scale of post-disaster services to local health systems will never be sufficient nor sustainable without addressing systems-level problems.
References
- Bischoff, R.J., Springer, P.R., Taylor, N. (2017). Global Mental Health in Action: Reducing Disparities One Community at a Time. Journal of Marital and Family Therapy, 43, 276-290. doi: 10.1111/jmft.12202
- Kirmayer, L.J., Pedersen, D. Toward a new architecture for global mental health. Transcultural Psychiatry. 2014;51(6):759-776. doi: 10.1177/1363461514557202
- North, C.S. Pfefferbaum, B. Mental Health: Response to Community Disasters: A Systematic Review. JAMA. 2013;310(5):507-518. doi: 10.1001/jama.2013.107799
- Jordans, M., & Kohrt, B. (2020). Scaling up mental health care and psychosocial support in low-resource settings: A roadmap to impact. Epidemiology and Psychiatric Sciences, 29, E189. doi:10.1017/S2045796020001018
- Lund C, Brooke-Sumner C, Baingana F, Baron EC, Breuer E, Chandra P, Haushofer J, Herrman H, Jordans M, Kieling C, Medina-Mora ME, Morgan E, Omigbodun O, Tol W, Patel V, Saxena S. Social determinants of mental disorders and the Sustainable Development Goals: a systematic review of reviews. Lancet Psychiatry. 2018 Apr;5(4):357-369. doi: 10.1016/S2215-0366(18)30060-9.
- Bredström, A. Culture and Context in Mental Health Diagnosing: Scrutinizing the DSM-5 Revision. J Med Humanit 40, 347–363 (2019).
- Raviola G, Eustache E, Oswald C, Belkin GS. Mental health response in Haiti in the aftermath of the 2010 earthquake: a case study for building long-term solutions. Harv Rev Psychiatry. 2012;20(1):68-77. doi:10.3109/10673229.2012.652877
- Semrau, Maya, et al. “Strengthening Mental Health Systems in Low- and Middle-Income Countries: The Emerald Programme.” BMC Medicine, vol. 13, no. 1, 10 Apr. 2015, 10.1186/s12916-015-0309-4. Accessed 7 May 2019.
- Epping-Jordan, JoAnne E, et al. “Beyond the Crisis: Building Back Better Mental Health Care in 10 Emergency-Affected Areas Using a Longer-Term Perspective.” International Journal of Mental Health Systems, vol. 9, no. 1, 12 Mar. 2015, 10.1186/s13033-015-0007-9. Accessed 13 June 2020.
About GEMSLP project proposals
These project proposals are completed by our mentees, who are medical students, to encourage independent thinking from a global perspective.
Thank you to our authors and presenters!

Alison Neely, MS4
Albert Einstein College of Medicine

Luxi Qiao, MS4
Washington University School of Medicine
Jacob Reshetar, MS4
University of Minnesota School of Medicine
Blog Editorial Team

Halley Alberts, MD
PGY-2 University of South Carolina Prisma Health Midlands
Co-Director & Blog Editor

Jeff Downen, MD, MS
PGY-2 University of Florida, Jacksonville
Blog Editor

Mohamed Hussein, MBBCh
Trauma Research Fellow
Blog Editor
Keep in Touch:
Sharing is caring
- Share on X (Opens in new window) X
- Share on Reddit (Opens in new window) Reddit
- Share on LinkedIn (Opens in new window) LinkedIn
- Share on Facebook (Opens in new window) Facebook
- Share on Tumblr (Opens in new window) Tumblr
- Share on Pinterest (Opens in new window) Pinterest
- Share on WhatsApp (Opens in new window) WhatsApp
- Email a link to a friend (Opens in new window) Email
- Print (Opens in new window) Print

