Epidural Hematoma
Authors: Kilalo Maeli Mjema, Emergency Physician and Mugisha Clement, Neurosurgeon.
Case Presentation
A 34 years old male sustained a traumatic brain injury following a motor vehicle accident 3 hours before presentation to ED. BP: 117/69mmHg. HR: 84, RR: 18, SPO2: 99% in room air, T: 36.9.
Primary Survey
Airway: patent and protected
Breathing: bilateral equal air entry
Circulation: warm extremities, 1 second capillary refill time
Disability: alert and oriented, pupils 4mm bilaterally equally reactive to light, RBG 5.6 mmol/L
Exposure: raccoon right eye, bruises on the forehead and upper limbs
SAMPLE History
Signs and symptoms: mostly chest pain than the headache, nausea
Allergies: no known allergies
Medication: had received tramadol, dexamethasone, tetanus toxoid and some intravenous fluids before being referred to our facility
Past medical history: no known comorbid or any significant history
Event: sustained motor vehicle accident as a motorcycle driver with no helmet on 3 hours prior presentation, associated with a 20 minutes loss of consciousness. Attended at another facility where he regained his full consciousness, wounds dressed, medication given as above, E-FAST negative and CT imaging done. He remained conscious throughout and was transferred for neurosurgical observation and interventions.



Neuro-observation and continuous monitoring were planned. Blood samples sent for CBC, PT, aPTT, blood type and crossmatch. The neurosurgical review was done, and the patient was to be kept inpatient for close neurosurgical observation and interventions as needed.
Patient progress while still in the ED
In the course of stay in the ED, the patient started to vomit, became drowsier overtime, was moving mostly the right side of his limbs. The right pupil was 6-7mm non-reactive to light and GCS dropped to E1M4(Rt)V2
Vitals
BP 133/79 mmHg HR 39-45 bpm RR 14 rpm SPO2 99% in room air.
The patient was emergently transferred for repeat imaging and prepared for emergency craniotomy and hematoma evacuation. Theatre was informed and ready to receive the patient.
Rapid sequence induction and intubation
- Patient pre-oxygenated
- Induction with iv ketamine 2mg/kg (weight 75kg)
- Paralyzed with iv suxamethonium 100mg
- Intubated by sized 8 cuffed ETT

Mannitol 20g iv infusion was given over 10 minutes.
Intraoperative Findings and Progress
Right frontotemporoparietal craniotomy was done. Approximately 100 mls of hematoma because of spurting bleeding from the medial meningeal artery was found. No other obvious identifiable bleeding was seen. Hemostasis was achieved and closed in layers with a drain. The patient had a complete neuro improvement, extubated at day 5 and discharged 9th day.
Clinical Pearls
- The incidence of epidural hematoma is highest among adolescents and young adults
- Most cases are a result of head trauma by traffic accidents, falls or assaults
- Most commonly due to middle meningeal arterial bleed
- Epidural hematoma does not cross suture margins but crosses dural attachments as a convex lens shaped appearance
- Lucid intervals are seen in patients
- Watch for raised intracranial pressure; ipsilateral dilated pupil, Cushing reflex, altered mentation, vomiting
- Glucocorticoids have no role in reducing cerebral edema in traumatic brain injury
- In the presence of epidural hematoma with the feature of herniation, mannitol can be given with caution that craniotomy and evacuation is going to be done immediately
- Ketamine in RSII can still be considered in traumatic brain injury where blood pressures are not raised
Clinical Pearls
In the context of non-operative management, properly monitoring neurologic status and progress is the key factor to recognise early need of emergency medical intervention, re-imaging and neurosurgery.
References and Further Reading
- Bullock MR, Chesnut R, Ghajar J, et al. Surgical management of acute epidural hematomas. Neurosurgery 2006; 58:S7.
- Besenski N. Traumatic injuries: imaging of head injuries. Eur Radiol 2002; 12:1237.
- Matsumoto K, Akagi K, Abekura M, Tasaki O. Vertex epidural hematoma associated with traumatic arteriovenous fistula of the middle meningeal artery: a case report. Surg Neurol 2001; 55:302.
- Heit JJ, Iv M, Wintermark M. Imaging of Intracranial Hemorrhage. J Stroke 2017; 19:11.
- Roberts I, Yates D, Sandercock P, et al. Effect of intravenous corticosteroids on death within 14 days in 10008 adults with clinically significant head injury (MRC CRASH trial): randomised placebo-controlled trial. Lancet 2004; 364:1321.
- Nath F, Galbraith S. The effect of mannitol on cerebral white matter water content. J Neurosurg 1986; 65:41.
- Baekgaard JS, Eskesen TG, Sillesen M, et al. Ketamine as a Rapid Sequence Induction Agent in the Trauma Population: A Systematic Review. Anesth Analg 2019; 128:504.
Sharing is caring
- Share on X (Opens in new window) X
- Share on Reddit (Opens in new window) Reddit
- Share on LinkedIn (Opens in new window) LinkedIn
- Share on Facebook (Opens in new window) Facebook
- Share on Tumblr (Opens in new window) Tumblr
- Share on Pinterest (Opens in new window) Pinterest
- Share on WhatsApp (Opens in new window) WhatsApp
- Email a link to a friend (Opens in new window) Email
- Print (Opens in new window) Print
The Pediatric patient in the ED: Peculiar and Paramount
Children are not young adults!
This was the opening speech of the first Pediatrics lecture in my medical school.
As Emergency Physicians, we deal with everything and everyone at the same time; in some instances, the segmentation between types of patients blurs. The pediatric patient in the middle might be a challenge if you are not working in an independent Pediatrics Emergency Department.
In some situations, you will have to make decisions by conscious contemplation rather than pattern matching, which we mostly depend on in our approach.
Having had the privilege of working in an independent Pediatrics ED, I realized how much easier decision making becomes when you have a set of mind prepared to deal with a child.
Health problems for children differ from those of adults. A child’s response to disease and stress varies with age and development; therefore, it’s fundamental to approach children in a way that identifies and tackles the differences.

Judge by appearance
We use heuristics frequently in our practice, perhaps the most popular among which is the (sick/not sick) paradigm. When it comes to children, appearance is of particular importance.
The look might be deceptive in adults, but it’s not the case in children; as they say, the eyes don’t lie, but it can be lied to.
For its virtual implication, appearance represents the first component of the Pediatrics assessment triangle, our quick and orderly assessment tool for children.
Power and authority
Children can’t consent or advocate for themselves, a parent or legal guardian approval is required to deliver health care. The most notable exception to this is the emergency situation, in which consent is not required, and care can be delivered if parents are not present and even against their wishes. The emergency situation gives the emergency physician the highest authority in decision making in children, which is a titanic responsibility.

The Math geek
Dosing for most medications in children is weight dependent. It might be good practice for your brain but can also represent a dilemma if you are giving verbal orders and your phone is not with you. My colleague once said I was terrible at Math; that’s why I went to medical school; I think she made a good point.
Baby shark
ED is a noisy environment, but the Pediatrics ED is on another level of noise. Other than natural sounds found in the ED and crying fussy children, you will also encounter countless children’s music and disturbing games. It might sound nihilistic and resentful, but I have to be forthright, the current children’s entertaining materials lack educational value and taste, and it needs resuscitation.

Priceless outcome
In the end, the smile on a child’s face is one of the most satisfying experiences ever and a blessing. Establishing a rapport with a child is the key to a proper exam. Children won’t trust anything that’s not genuine, and care should be delivered with love and passion. You might also need to learn some tricks and give some treats to accomplish that, in the hope that you reach the fruitful outcome of drawing a smile on God’s angelic creatures.
Sharing is caring
- Share on X (Opens in new window) X
- Share on Reddit (Opens in new window) Reddit
- Share on LinkedIn (Opens in new window) LinkedIn
- Share on Facebook (Opens in new window) Facebook
- Share on Tumblr (Opens in new window) Tumblr
- Share on Pinterest (Opens in new window) Pinterest
- Share on WhatsApp (Opens in new window) WhatsApp
- Email a link to a friend (Opens in new window) Email
- Print (Opens in new window) Print
Acute Management of Supraventricular Tachycardias
The term “supraventricular tachycardia (SVT)” expresses all kinds of rhythms that meet two criteria: Firstly, the atrial rate must be faster than 100 beats per minute at rest. Secondly, the mechanism must involve tissue from the His bundle or above. Mechanism-wise, atrial fibrillation resembles SVTs. However, supraventricular tachycardia traditionally represents tachycardias apart from ventricular tachycardias (VTs) and atrial fibrillation (1,2).
Supraventricular tachycardias are frequent in the ED!
The SVT prevalence is 2.25 per 1000 persons. Women and adults older than 65 years have a higher risk of developing SVT! SVT-related symptoms include palpitations, fatigue, lightheadedness, chest discomfort, dyspnea, and altered consciousness.
How to manage supraventricular tachycardia?
In clinical practice, SVTs are likely to present as narrow regular complex tachycardias. Concomitant abduction abnormalities may cause SVTs to manifest as wide complex tachycardias or irregular rhythms. However, 80% of wide complex tachycardias are VTs. Most importantly, SVT drugs may be harmful to patients with VTs. Therefore, wide complex tachycardias should be treated as VT until proven otherwise (1,2).
The chart below summarizes acute management of regular narrow complex tachycardias:

References and Further Reading
- Brugada, J., Katritsis, D. G., Arbelo, E., Arribas, F., Bax, J. J., Blomström-Lundqvist, C., … & Gomez-Doblas, J. J. (2019). 2019 ESC Guidelines for the management of patients with supraventricular tachycardia: the Task Force for the management of patients with supraventricular tachycardia of the European Society of Cardiology (ESC). European Heart Journal, 00, 1-66.
- Page, R. L., Joglar, J. A., Caldwell, M. A., Calkins, H., Conti, J. B., Deal, B. J., … & Indik, J. H. (2016). 2015 ACC/AHA/HRS guideline for the management of adult patients with supraventricular tachycardia: a report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines and the Heart Rhythm Society. Journal of the American College of Cardiology, 67(13), e27-e115.
Sharing is caring
- Share on X (Opens in new window) X
- Share on Reddit (Opens in new window) Reddit
- Share on LinkedIn (Opens in new window) LinkedIn
- Share on Facebook (Opens in new window) Facebook
- Share on Tumblr (Opens in new window) Tumblr
- Share on Pinterest (Opens in new window) Pinterest
- Share on WhatsApp (Opens in new window) WhatsApp
- Email a link to a friend (Opens in new window) Email
- Print (Opens in new window) Print
Hyperkalemia Treatment – Infographic

Further Reading
Weisberg LS. Management of severe hyperkalemia. Crit Care Med. 2008 Dec;36(12):3246-51. doi: 10.1097/CCM.0b013e31818f22b. Review. PubMed PMID: 18936701.
Sharing is caring
- Share on X (Opens in new window) X
- Share on Reddit (Opens in new window) Reddit
- Share on LinkedIn (Opens in new window) LinkedIn
- Share on Facebook (Opens in new window) Facebook
- Share on Tumblr (Opens in new window) Tumblr
- Share on Pinterest (Opens in new window) Pinterest
- Share on WhatsApp (Opens in new window) WhatsApp
- Email a link to a friend (Opens in new window) Email
- Print (Opens in new window) Print
Why Me? The Story of My Burnout – Part 3
The story continues from link (Part 2).
I must take a deep breath. I must ask for help.
The Self-Knowledge Path
I could go away and work in another hospital. We have many good hospitals in Brazil. Some even employ emergency physicians who are local graduates. I really could. In truth, there would be no shame if I left the hospital. But I decided to give it one more try.
I just want to make clear that there is no single route back from burnout. It is a multifactorial treatment. You need emotional power. Some you may already have, or you can develop with a mental health specialist’s help. Some you will gather alone, or family and friends will help you to recover if you are lucky enough. Read, talk, discuss, and share with your community. You will never be alone because it is the system that is inflicting moral injury and burning you, and everybody, out.
Each person needs different means and tools to recover. We have to acknowledge that not everybody can afford all of them. Not everybody can pay for a therapist or even leave their work. I was one of the lucky ones. I could.
I promised myself and others that I would get better, and I wouldn’t give up. I felt obliged to improve the system that had harmed me. The system that made me afraid; afraid that I would fail.
It was not easy! It wasn’t “just not thinking about it.” It wasn’t “just a phase.” It wasn’t “just yoga.” It wasn’t “just wanting.” It was more than all the above. It took a long journey of self-knowledge: Who was I? What did I want? How could I achieve that?
Gradually, intertwined with relapses, the healing process began. I returned to therapy. Thanks to all support from my amazing friends, -virtual friends, present friends, distant friends- mentors, mentees, students, residents, followers, I was overwhelmed with affection and understanding. There were messages of encouragement everywhere I looked and listened. I did not plan this. It happened organically from across our community, and sometimes unintentionally, as I reached out to others, who always found time to help me.
Kindness can save a life! If you feel so, just go around saying how important people are in your life. I assure you that the kindness and positive comments of these people saved me.
I improved gradually in small steps. With empathy and determination, I took one step after another. Each step led me to find new perspectives. With each small victory, I felt a small but important celebration in my heart.
Yet, I wanted to make sense of it all. How to endure the moral injury? How to continue working here? I desperately needed to make sense of my job.
Why Me?

In addition to therapy, I went on leave. I flew away and spent time in Mozambique, an LMIC, with many more difficulties, compared to Brazil. They were just beginning to develop the first emergency medicine residency program, and they had a lot more work to do. They were seemingly starting from scratch, and they had fewer resources than we had in Brazil. I found their enthusiasm and resourcefulness more inspiring than I thought possible.
It wasn’t because I could see how lucky we are in Brazil, but they did their best even though they were aware of their problems. I knew that there was no way that I could give up after seeing them.
I returned to Brazil, where people were eager to work with me. I felt they had missed me. They showed me that I made a difference.
I was fortunate to see my work environment improved. The administration had started to ‘get it,’ and now they cared about what we do. They realized that efficient systems saved money, so they were helping us achieve better care for our patients. Our department was renovated. They hired more people, and we got better medications. It all helped. It felt as though they were listening.
So recovering from burnout not only helped me to accept that problems are a part of the system but also made me realize people make the system. Therefore we can change it to accommodate our needs. Not the contrary. We need to END moral injury by addressing it and demanding solutions! We don’t need to be resilient to it!
In the beginning, I understood that I needed to be present in all my tasks, but that’s a challenge in the hectic world of emergency medicine. In truth, we are not as good at multitasking as we let ourselves think. However, we get better at prioritizing and scheduling tasks as we develop as clinicians. More importantly, we learn to give each task the proper time and attention it deserves.
As time passed, my most challenging feelings diminished. I redefined my responsibilities and my choices, redefined my motivation, my ambition, my purpose. I adjusted my expectations. I found a new power.
Then, gradually, the love for Emergency Medicine and the energy to become the doctor I aspire came back. However, I still had to face my demons and deal with the most painful side of emergency medicine: Delivering bad news.
“Most of the time, the fact that you care is enough” is one of the most effective pieces of advice that I ever received. It helped me relieve the intense pain that I didn’t even know it was there. I still remind others and myself of it regularly.
For example, I dealt with the tragic case of pediatric cardiac arrest, brought in by another medical team. We did CPR over an hour, as this was a very delicate situation with a child. At the debriefing, I was careful with both teams from the other hospital and our own. Although I was worried about having the conversation I did, I was shocked and stunned to hear the reply. The doctor shrugged and said:
– Yeah, right. Can I go now?
He was in a rush. He didn’t even want to hear the debriefing. He didn’t appear to care! The disdain broke my spirit, and the whole team felt the same anger. It made everything harder to cope.
I took a deep breath, thanked the team for all the effort, asked them to prepare the body, and went to the waiting room to talk once again with the father. I had been there a lot of times, talking through everything as we were trying to resuscitate, so he already knew me, and immediately recognized my expression of bad news. I sat next to him and told him everything we did. I was trying to remedy the anguish while allowing time for understanding.
– There was nothing more we could do. I’m so sorry, but he died.
The father stared at the floor for a while.
– My wife is eight months pregnant. What should I do now?
He was in despair. Next came tears. I waited. Present. Then, he looked at me with honest:
– Thank you, doctor, for everything you did.
I will never forget them.
“Most of the time, the fact that you care is enough.”
I can’t stop people from getting sick. I can’t even guarantee who will survive, much less, meet the expectations of families. I can’t fix all the system by myself. Yet, I can show that we care, which is now my purpose and mantra.
Now, when I have to deliver bad news, I try my best to be there and look in the eyes. I patiently wait to make sure until there is no doubt. I don’t try to hide my feelings, and I finally feel I’m always telling the truth:
– We are doing everything we can.
I ensure that they know we care. I make a difference there. My pain eases as theirs alleviates even a little.
“Most of the time, the fact that you care is enough.”
I can’t stop people from getting sick. I can’t even guarantee who will survive, much less, meet the expectations of families. I can’t fix all the system by myself. Yet, I can show that we care, which is now my purpose and mantra.
Finding My Ikigai

Ikigai is a Japanese concept that means “a reason for being.” In English, the word roughly means “thing that you live for” or “the reason for which you wake up in the morning.” Each individual’s ikigai is personal and specific to their lives, values , and beliefs. It reflects the inner self and faithfully expresses that, while simultaneously creating a mental state in which the individual feels at ease.
The thing I like most about ikigai is that it is for everyone. You have to understand yourself to achieve this deeply. Seeking self-knowledge can be the most challenging part.
– Am I doing something that I love?
– Am I doing something that the world needs?
– Am I doing something that I am good at?
– Am I doing something that I can be paid for?
YES!
So, where am I now?
Well, I still love heart attacks! I love the look of amazement of the interns when we save a life. I love the self-satisfaction of the residents when they can do something correctly for the first time. I love how happy the team gets when we can do perfect resuscitation. I love the peculiarities of each patient, their life, culture, and beliefs. I love to learn something new every day. And that’s why Emergency Medicine!
I love heart attacks! But when we can't save, when the system fails, when the patient dies but I feel that I softened the pain, even a little bit, by showing that we care, I know I can endure.
And that's why, me.
Sharing is caring
- Share on X (Opens in new window) X
- Share on Reddit (Opens in new window) Reddit
- Share on LinkedIn (Opens in new window) LinkedIn
- Share on Facebook (Opens in new window) Facebook
- Share on Tumblr (Opens in new window) Tumblr
- Share on Pinterest (Opens in new window) Pinterest
- Share on WhatsApp (Opens in new window) WhatsApp
- Email a link to a friend (Opens in new window) Email
- Print (Opens in new window) Print
Why Me? The Story of My Burnout – Part 2
The story continues from link (Part 1)
I had already been tired and sad. Now, I was also feeling wronged.
The Dangers of Burnout
It meant that heart attacks stopped being exciting. I started to resent them as they now caused me to suffer. I have nowhere else to refer the patient, or the specialty doctors criticized me.
They mistreated me, perhaps because of a lack of trust, or they too were damaged by the system. Maybe it was about payments and expenses. I did not know, but the effort of constant fighting was exhausting.
The system hit me hard. It was clear: irritation, stress, discontent, three quarrels with my team and my superiors in one week. I was burned out. That was putting my good work at risk.

I felt like everything I was doing was meaningless. I aspired to become the best possible doctor through studying, traveling and sharing, but I always returned to the conditions that made me feel that all was in vain. My stagnant environment was full of burnout people, unjust deaths and endless problems regarding insufficient resources versus higher and higher demand.
That saddest thing in medicine is a doctor without hope.
I felt that each patient brought more pain than joy, even when we had excellent outcomes. It made me sick. I felt like I had unlearned hope. To make matters worse, I could not contain these emotions.
One day a patient asked me, “Am I going to die, doctor?”
I had just seen the results. It suggested cancer, but what would happen now? We wanted an expert to lead him, necessitating an evaluation by the oncologist. Still, the oncologist would not see the patient until the biopsy result, despite the imaging strongly suggested cancer. That meant we had to ask the general surgeon to do the biopsy, but in return, he asked us to refer the patient to another surgical specialty, based on the location of the tumor. So we tried, but this type of specialist did not serve in our region.
The patient’s and our growing stress and conflict eventually led the general surgeon to do the biopsy, but the patient had to wait 30 to 45 more days for the result. Only then, he would be able to go back to the oncologist. When he did, tho oncologist asked us for phenotyping. One more week passed until we finally get the patient to oncology, only to be declared too sick for treatment.
I had experienced this so many times before. Meanwhile, patients were getting more sick, and repeatedly ended up in the emergency department, sometimes got admitted, only to treat infections or pain. In the end, they were sent by the internist to die in our emergency room. They could not do end-of-life care properly. I frequently talked to an enraged family, not because of cancer, but because they were led to believe there was a chance of treatment.
My opinion is that the problem wasn’t lying to the patient about cure cancer, but how often the system don’t even give them this chance of a fight, lying about a chance to treat, but in really being just harmful for everybody because disorganization, corruption, and for didn’t care.
We do not cure death. Ever.
Sometimes we can prolong life. We hope for a good life with meaning, so that they can enjoy some more years, months, weeks or days of celebration, and prepare their wishes for a decent death with their family.
My opinion is that this realization is important not only when we talk about cancer, but any condition, even like a heart attack. We do not cure death, ever.
Coming back to that new patient, the words and the questions bounced in my head:
– Am I going to die, doctor?
– Don’t think about it now. We will take care of you.
I don’t know what the patient saw in me. To me, It felt like lying. When I said we would do our best, it wasn’t me but the system lying. Even if we as emergency physicians or I as an individual did everything possible, I felt the system didn’t care. I knew the system could do better. What could I say when I knew that the journey I want for my patients is so unachievable in the system I work in. I no longer knew what to say under these circumstances, and I felt the patient recognized that in my soul.
I felt hurt, guilty, beaten, and bitter.
That saddest thing in medicine is a doctor without hope.
I never thought this could happen to me. Not with me! How could this happen to me? I was in love with Emergency Medicine! Wasn’t I?
I’d said a billion times how I loved Emergency Medicine and didn’t know how to live without it. I’d shared my passion, convincing others that Emergency Medicine was the answer. Now, it felt like Emergency Medicine was killing me. And worst, I felt that I was not doing good for my patients as my lies were hurting them.
I must take a deep breath. I must ask for help. ...to be continued...
Sharing is caring
- Share on X (Opens in new window) X
- Share on Reddit (Opens in new window) Reddit
- Share on LinkedIn (Opens in new window) LinkedIn
- Share on Facebook (Opens in new window) Facebook
- Share on Tumblr (Opens in new window) Tumblr
- Share on Pinterest (Opens in new window) Pinterest
- Share on WhatsApp (Opens in new window) WhatsApp
- Email a link to a friend (Opens in new window) Email
- Print (Opens in new window) Print
iEM Monthly – January 2020

Recent News
iEM was viewed more than 100.000 by over 60.000 visitors in 2019. Our resources reached to 197 countries. The first edition (2018) of free Emergency Medicine Clerkship Book has been downloaded over 4000 times. During 2019, we continuously published posts written by 29 blog authors. We thank all contributors and followers and wish you all a happy new year.

Inside iEM
Two new blog authors joined us in December 2019. We welcome Dr. Israa M. Salih from UAE and Dr. Nadarajah Prasanna from Sri Lanka.

Sri Lanka
Senior registrar in emergency medicine at Postgraduate Institute of Medicine, University of Colombo. Full instructor for European Resuscitation Council ALS courses as well as local APLS and NLS courses. Completing the Full instructor pathway for International APLS and ATLS courses by 2020. Interested in resuscitation, pediatric emergency medicine, simulations and MEdED. Currently involved in teaching resuscitation courses as well as diploma in emergency nursing , EMT refresher course and medical student teaching.

UAE
EM resident in ZMH, Abudhabi. Served in human rights and peace office IFMSA | Advocate of FOAM | Profound interest in research, critical care and disaster medicine | Also a poet and part-time philosopher.
Recent Posts
Top Countries
These countries viewed iEM content the most in 2019.

What is iEM
Sharing is caring
- Share on X (Opens in new window) X
- Share on Reddit (Opens in new window) Reddit
- Share on LinkedIn (Opens in new window) LinkedIn
- Share on Facebook (Opens in new window) Facebook
- Share on Tumblr (Opens in new window) Tumblr
- Share on Pinterest (Opens in new window) Pinterest
- Share on WhatsApp (Opens in new window) WhatsApp
- Email a link to a friend (Opens in new window) Email
- Print (Opens in new window) Print
Why Me? The Story of My Burnout – Part 1
This story starts like almost every other: I fell in love.
The thing is, I LOVE heart attacks!
I know this is a weird statement, maybe even a little overstated. I know that people can get uncomfortable when I say this. When I said it for the first time, full of enthusiasm and with sparkling eyes, my ex-fiance looked at me in a concerned and puzzled way: ‘Can you say that?’ – He asked, wondering if it was appropriate for a doctor to say that they actually enjoyed the experience of people being so unwell.
Clearly, as a doctor, I have nothing against people. Quite the contrary, I unceasingly fight for them to survive and thrive. Yet the paradox is real, despite my battle to save my patients, I am so in love with heart attacks!
Why? Perhaps I love the puzzle behind it. When the patient arrives, I see the position of the body, the hand on the chest, fingers tightly pressed against the skin, the skin color, the sweating… I consider the nuances of pain types, the comorbidities, the risk factors… All are informing my judgment and decisions even before I get to look at the ECG.
I love knowing the diagnosis as it reveals itself. I love that I can treat it. And when it works, I’m the queen of my craft. The scores of survival game change. 1 for me, 1 for my patient, and 0 for the heart attack!
So that’s why you would see me so happy when a patient arrives in my ED. I love this feeling. I love this adrenaline rush that is emergency medicine and me! I love leading a code, guiding actions, organizing my team to the point of ROSC. I love that roaring energy that runs through the whole team as we effortlessly move to the next stage of resuscitation.
This is why I love Emergency Medicine.
Emergency Medicine is new In Brazil. The general assumption is that ED is where junior physicians serve until they choose another specialty or other specialists work to earn additional income. Until recently, working in the ED was a difficult job with no career advancement. So, when I realized that I was so in love with more than heart attacks that I could not leave my work as an Emergency Physician, people started to ask me, “Are you sure? Do you want to work forever in an ED in Brazil? What about when you get older? Don’t you think you will get tired and burned out?”

I don’t think so. I reply, “I love my job. When you love your job, you don’t ever get tired.”
How naive I was.
Emergency medicine is tough, sometimes even painful. Deaths, we can’t help. Diagnoses of incurable diseases. Bad news. The pressure to be good, perfect, productive. Adding to that, many of us work in corrosive health systems: The result? Emergency Medicine can burn you to your core.
Being in love with Emergency Medicine is enough to protect us?
Emergency Medicine can burn you to your core.
Leaving the Comfort Zone
I am a curious soul. While I learned more about emergency medicine, I discovered another world with worldwide Emergency Physicians, who could understand my difficulties and help me learn remotely from them. I fell in love again with #FOAMed.
Hearing the experiences of my colleagues from all around the world inspired me to travel and meet those people. I wanted to learn with them and to compare how Emergency Medicine is in those places.

My newly found calling took me to Sydney in Australia, such a lovely country, which had beautiful and polite people, good public transportation, beautiful scenery, and even a public healthcare system too!
I was lucky enough to spend time in an excellent hospital in NSW. I witnessed them receiving a trauma patient and listened to them as they plan patient management. I was speechless. I felt a sudden sadness to the degree that I wanted to crawl back to my mother’s womb.
When I tell this story, people often react, “You don’t need fancy stuff to practice Emergency Medicine,” but it was not what I saw there. What was it? It wasn’t the video laryngoscopy. It wasn’t the infinite bougies and disposable LMAs. That’s true: The facilities in Australia were incredible and so much more were available than back home in Brazil. But it was still the people.
When the paramedic team arrived, the whole team discussed the patient plan. They were so courteous and respectful to each other, focused only on doing the best for the patient. They were excited about the case, energized, and happy for doing their best.
I’m not saying their life is easy. I’m not saying they don’t suffer moral injury. But I’m sure they don’t show ill-will to their peers and most importantly, to their patients. I want so badly to be able to do that kind of medicine, but the realization of this new health system made me feel envious and perhaps even hopeless. Their experience was so positively different from mine.

I spent the next day in my room, lying depressed in bed, staring at the ceiling, trying to figure out what to do now: “How I would love to have that experience in my hospital!”
I thought a lot about what happened there. Why did it hit me so hard? I knew that not all hospitals were the same in Australia as some hospitals had problems and struggles like in Brazil. I already knew that we had hospitals in Brazil better than mine. Why did I feel so hopeless then?
Now, looking back, I can understand better. I was pushing my comfort zone further than I ever did in my entire life. I was discovering a lot about myself and my capabilities. I was achieving success through FOAM. And so, I saw my limitations, I strumbled in a deep Impostor Syndrome and lost some excellent opportunities. I was in such a fragile mindstate that I felt like the system was unfair to me.

In my hospital, which is always overcrowded, I work with physicians that don’t have the mindset of Emergency Medicine. When a trauma patient arrives, it feels like a battle. Physicians challenge paramedics: “Why did you bring this patient here when we don’t have bed enough?” or “we don’t have enough surgeons!” or “why does nothing here work?”
All too frequently, the team ends up shouting at each other.
I tried hard to spread the ideas and visions I was learning. One time, I asked for an ultrasound machine, my boss laughed in my face: “Where do you think you are?” Everybody seemed so consumed by pessimism and fatigue that they lost all hope.
I had already been tired and sad. Now, I was also feeling wronged. ...to be continued...
Sharing is caring
- Share on X (Opens in new window) X
- Share on Reddit (Opens in new window) Reddit
- Share on LinkedIn (Opens in new window) LinkedIn
- Share on Facebook (Opens in new window) Facebook
- Share on Tumblr (Opens in new window) Tumblr
- Share on Pinterest (Opens in new window) Pinterest
- Share on WhatsApp (Opens in new window) WhatsApp
- Email a link to a friend (Opens in new window) Email
- Print (Opens in new window) Print
Epistaxis on a Flight
A couple of days ago, a friend told me about an incident that had occurred on a plane where a middle-aged man was found to have epistaxis (bleeding from the nose) midway between a 4-hour flight. Although epistaxis has various degrees of severity and only a small percent are life-threatening, the sight of blood, no matter the amount, is a cause of panic and anxiety for everyone. Hence, the cabin crew was called and helped in managing the patient until the flight landed.
Some of the causes of epistaxis on a flight are dryness in the nose due to changes in cabin pressure and air conditioning. Other causes depend on patients’ previous health problems, which may include medications such as warfarin, bleeding disorders, nose-picking.
As important as it is to learn the emergency management of epistaxis in a hospital setting, often you come across a scenario such as this, in your daily life and its essential to know how to manage it, out of the hospital setting or even in the emergency department, while taking history or waiting to be seen.
The following are a few steps you can take for initial conservative management of epistaxis:
- Make sure they are breathing normally and not in any distress, asses their condition and if you think this could be a major emergency, contact the doctor or call for an ambulance
- Ask them to bend forward toward their waist while sitting up (to prevent swallowing of blood)
- Place cotton wool or tissue into the bleeding part of the nose
- Pinch the soft part (alae tightly against the septum) of the nose just above the nostrils for 10-15 minutes
- Blowing the nose to expel blood and clots
- Additionally, an ice pack can be pressed on the bridge of the nose to stop bleeding
If the following measures fail, further medical management may be advised.
Overview
Epistaxis is acute hemorrhage from the nose, nostrils, nasopharynx, and can be either anterior or posterior, depending on the source of bleeding. It is one of the most common Otolaryngological Emergencies.
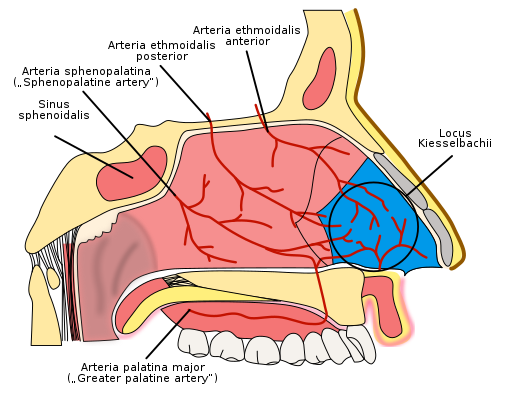
Anterior bleeds are the most common, and a large proportion is self-limited. The most common site is ‘Little’s area’ also known as Kiesselbach’s plexus (Anastomosis of three primary vessels occurs in this area: the septal branch of the anterior ethmoidal artery; the lateral nasal branch of the sphenopalatine artery; and the septal branch of the superior labial branch of the facial artery).
Posterior bleeds are less common and occur from posterolateral branches of the sphenopalatine artery and can result in significant hemorrhage.
Causes of epistaxis
Nose picking, dryness, allergic or viral rhinitis, foreign body, trauma, medications (anticoagulants), platelet disorders, nasal neoplasms, hereditary hemorrhagic telangiectasia (Osler-Weber-Rendu disease), aspirin.
Assessment and Management
- ABC approach is a standard. Fluid resuscitation in severe cases
- History: severity, duration, previous episodes, trauma, medications, family history, infections
- Initial conservative management: as mentioned earlier including spraying the nares with oxymetazoline
- Examination: mental status, signs of shock, and coagulopathy and examination of the nose
- Treatment options: Chemical cautery is usually performed with silver nitrate, Nasal Packing, Nasal Tampons, Gauze Packing, Nasal Balloon Catheters, Tranexamic acid, Thrombogenic foams and gels
- Treatment specific to posterior bleeds : Balloon catheter, Foleys catheter, Cotton Packing
References and Further Reading
Alter Harrison. Approach to the adult epistaxis. [December 24th, 2019] from: https://www.uptodate.com/contents/approach-to-the-adult-with-epistaxis
Sharing is caring
- Share on X (Opens in new window) X
- Share on Reddit (Opens in new window) Reddit
- Share on LinkedIn (Opens in new window) LinkedIn
- Share on Facebook (Opens in new window) Facebook
- Share on Tumblr (Opens in new window) Tumblr
- Share on Pinterest (Opens in new window) Pinterest
- Share on WhatsApp (Opens in new window) WhatsApp
- Email a link to a friend (Opens in new window) Email
- Print (Opens in new window) Print
A Song of Ice and Fire
As the year comes to an end, the holidays approach and, for lots of people, it means traveling to different places around the world. For those who live in the southern hemisphere, like me, the summer comes with al power, with temperatures as high as 35°C (95°F) or 40°C (104°F). For those who live in the northern hemisphere, “the winter is coming” and bring with him temperatures below 0°C (32°F) in some places. With these temperature extremes, we have some conditions to have in mind when working in the ED. How to treat a homeless patient who has slept on the streets on a freezing night? And how about an elderly person who lay on the beach sand under a blazing sun?
Hyperthermia
What is hyperthermia?
By definition, hyperthermia is a condition when there is a failure of the body’s thermoregulatory mechanisms to handle extrinsic and intrinsic heat. It’s common to see the expression “Heat-related Illness” to describe the conditions associated to the exposure to environmental heat.
Physiology
The heat-related illness (HRI) develops following a progressive pattern, divided in 3 phases [1].
- ACUTE PHASE:
- Activation of inflammatory mediators, especially in the blood vessels;
- Gastrointestinal tract hypoperfusion, leading to bacterial translocation
- Respiratory alkalosis due to hyperventilation
- ENZYMATIC PHASE:
- Coagulopathy, leading to a hypercoagulability state
- Endothelial injury and microvascular thrombosis
- All of this leading to disseminated intravascular coagulation (DIC)
- LATE PHASE:
- Liver dysfunction secondary to DIC
- Kidney failure due to dehydration and hypotension
- CNS lesions leading to cerebral edema and hemorrhage
- Cardiovascular dysfunction, worsening hypotension and causing vasoconstriction
Risk Factors
- Extremes of age
- Obesity
- Elevated humidity rate
- Lack of acclimatization and/or fitness
- Ambient temperature
- Dehydration
- Cardiovascular disease
- Drugs/medication (i.e alcohol, diuretics, amphetamines)
Categories of heat illness
- Minor Heat Illness:
- Heat cramps: Intermittent muscle cramps likely related to salt deficiency and muscular fatigue, although the exact mechanism is not well known.
- Heat Edema: Swelling of the feet and ankles typically in non-acclimatized people
- Heat Syncope: Similar to orthostatic hypotension, caused by the physiologic response to the heat: volume depletion, peripheral vasodilatation and a reduced vasomotor tonus. More common in elderly people.
- Prickly Heat: cutaneous rash caused by pores and sweat gland obstruction
- Heat Exhaustion:
- Occurs with a moderate elevation in the body core temperature (<40°C or 104°F) – RECTAL temperature is the most reliable method (even though is a level C evidence)
- Usually accompanied by symptoms related to conditions described in the Minor Heat Illness and other nonspecific symptoms like nausea/vomiting, weakness and headache
- DOES NOT PRESENT WITH ALTERED MENTAL STATUS
- Heat Stroke:
- Body temperature above 40° (104°F) WITH ALTERED MENTAL STATUS
- Target organ damage
- Usually dry and pale skin, however athletes can present with warm and wet skin
Management
- Primary, we need to proceed with the basic measures: secure airway, monitorize and place IV fluids in order to maintain a mean arterial blood pressure > 60 mmHg [2].
- The second step is to perform a rapid cooling, targeting a temperature <39°C (102°F) in the first 30 minutes. After reaching this goal, the active cooling should be stopped in order to avoid overshoot hypothermia
- Cold water immersion is the best method available (level C evidence) [3].
- Treat shivering with benzodiazepines if needed (avoiding extra heat generation)
- DO NOT USE ANTIPYRETICS, they are not effective in this scenario [4].
- Cold water immersion is the best method available (level C evidence) [3].
Disposition
- Patients with heat stroke should be admitted to a ICU to monitoring organ dysfunction, electrolytes disturbances and rebound hypothermia.
- Young and otherwise healthy patients with heat exhaustion can be discharged home
- Be aware for the risk of recurrent hyperthermia when considering discharge a patient (returning to the same ambient)
Hypothermia
What is hypothermia?
- Condition in which the body loses heat at a higher rate than its capacity in maintain the core temperature or elevate the heat production
- Clinically defined as unintentional decrease of body temperature below 35°C (95°F)
- In other settings, we can talk about “secondary hypothermia”, when the patient has an impaired thermoregulation due to a clinical condition such as hypothyroidism, ketoacidosis, malnutrition etc – In this article we will focus on accidental hypothermia, related to environmental exposure
Physiology
- Initially, the metabolic rate increases, peripheral blood flow is shunted towards vital structures, and shivering initiates to increase heat production
- If these compensations are not enough, the body temperature continues to drop, with the CNS being affected when it reaches 35°C (95°F).
- Cardiovascular: initial increase in heart rate and blood pressure; however, as core temperature declines, progressive bradycardia and hypotension occurs. In more severe hypothermia, myocardial irritability increases, leading to a high risk of arrhythmias.
- Oxygen consumption: At a temperature of 28°C (82°F), the oxygen consumption is decreased by 50%, leading to a protective effect in CNS and other vital organs – but just if it develops before asphyxia (there are several studies trying to better understand the role of hypothermia as a protective measure in cardiac arrest) [5].
Risk Factors
- Fatigue
- Sleep deprivation
- Rain, wind and water immersion
- Burn
- Extremes of age
- Trauma
- Alcohol
- Hypoglycemia
- Hypothyroidism
- Hyperthermia treatment (rapid cooling)
Classification
Stage 1: Mild Hypothermia
- Core temperature: 32 – 35°C (90 – 95°F)
- Initially presenting with tachycardia, hypertension, shivering and vasoconstriction
- Gradually develops ataxia, poor judgement, amnesia, apathy, dysarthria
Stage 2: Moderate Hypothermia
- Core temperature 28 – 32°C (82 – 90°F)
- Loss of shivering, lethargy, mydriasis, hyporeflexia, alterations in cardiac rhythm (Osborne J waves on EKG)
Stage 3: Severe Hypothermia
- Core temperature: 24 – 28°C (75 – 82°F)
- Hypoventilation, ventricular fibrillation, acid-basic disturbances, anesthesia, pulmonary edema
Stage 4: Profound Hypothermia
- Core temperature: below 24°C (75°F)
- Oliguria, fixed pupils, asystole, apnea, coma
- Curiosity: 13,7°C (56,7°F) is the lowest temperature registered at which CPR was performed with satisfactory results [6].
Management
- The first thing we need to do is to stop the cooling process
- Remove the environmental factor (take the patient out of the street, take off wet clothes etc.)
- Try stop heat loss, putting up barriers like warm clothes, blankets, sleep bags, etc
- Second step, we should identify the degree of hypothermia to guide our approach:
- For Mild hypothermia, besides the strategies described before, we need to offer calories (food and warm drinks), monitoring for at least 30 minutes and warm the trunk
- [F]or Moderate hypothermia, we also need to keep the patient laid down and still, start volume reposition with warm fluids (40 – 42°C/104 – 107°F), Avoid food and beverage.
- For Severe hypothermia: All the above and check for pulse and breathing – of pulse/breathing is absent, START CPR. – Consider transferring to a facility where ECMO is available
- ECMO is the best option for severely hypothermic patients without signs of life who do not respond to initial resuscitative efforts. It has been shown to improve neurologically intact survival (48% to 63% survival with ECMO, <37% without ECMO) [7].
- For Severe hypothermia: All the above and check for pulse and breathing – of pulse/breathing is absent, START CPR. – Consider transferring to a facility where ECMO is available
“Nobody is dead until warm and dead”
Patients with core temperatures of <28°C have decreased electroencephalographic activity and loss of brainstem and pupillary reflexes, all of which may mimic death. Because of that, the patient can not be considered “dead” until his body temperature reaches at least 32°C.
Some conditions allow us to presume death even in patients with body temperature below 32°C and no vital signs: obvious lethal injury (i.e. decapitation), frozen body, potassium > 12, avalanche victims with burial > 35min or airway packed with snow.
References and Further Reading
The primary reference for this article was the recently launched book: “Medicina em Áreas Remotas no Brasil” (Wilderness Medicine in Brazil): JULIANA R. M. SCHLAAD e SASCHA W. SCHLAAD, Medicina em Áreas Remotas no Brasil, 1ed, Barueri (SP), Manole, 2020
Other sources of information as numbered and referred in the text:
- Powers SK, Howley ET. Regulação de temperatura. In: Powers SK, Howley ET. Fisiologia do exercício: teoria e aplicação ao conhecimento e ao desempenho. 9ed. Barueri: Manole; 2017. p.261-281.
- Tran TP. Heat emergencies. In: Ma OJ, Cline DM, ed. Emergency medicine manual. 6th ed. McGraw-Hill, NY: 2004:564-565
- Becker J, Stewart L. Heat-related illness. Am Fam Physician. 2011;83(11):1325-1330
- Lipman GS, Eifling KP, Ellis MA, Gaudio FG, Otten EM, Grissom CK. Wilderness medical society practice guidelines for the prevention and treatment of heat-related illness: 2014 update. Wilderness Environ Med. 2014; 25:S55-S65
- Soar J, Perkins G, Abbas G, et al. European Resuscitation Council Guidelines for Resuscitation 2010 Section 8. Cardiac arrest in special circumstances: Electrolyte abnormalities, poisoning, drowning, accidental hypothermia, hyperthermia, asthma, anaphylaxis, cardiac surgery, trauma, pregnancy, electrocution. Resuscitation. 2010;81(10):1400-1433.
- M. Gilbert, R. Busund, A. Skagseth, Nilsen PÅ, J.P. Solbø Resuscitation from accidental hypothermia of 13.7 degrees C with circulatory arrest Lancet, 355 (2000), pp. 375-376
- Brown DJ et al. Accidental hypothermia. NEJM 2012; 367(20): 1930-1938. PMID: 23150960
Sharing is caring
- Share on X (Opens in new window) X
- Share on Reddit (Opens in new window) Reddit
- Share on LinkedIn (Opens in new window) LinkedIn
- Share on Facebook (Opens in new window) Facebook
- Share on Tumblr (Opens in new window) Tumblr
- Share on Pinterest (Opens in new window) Pinterest
- Share on WhatsApp (Opens in new window) WhatsApp
- Email a link to a friend (Opens in new window) Email
- Print (Opens in new window) Print
Salter-Harris Fractures
Case Presentation
You are a medical student doing your first clinical shift as part of your Emergency Medicine rotation. A 9-year-old boy is brought in by his father after an injury to his left hand approximately 1 hour back. As explained by the father, the child was playing at home with his elder brother when his left index finger became caught in between a door that had quickly slammed shut. Following the injury, the child was reported to be crying due to severe pain, but had no lacerations or other associated injuries. He was rushed to the hospital and presented in the ED as an anxious, weeping boy who held out his left index finger and pointed to the tip as the region of maximal pain. Mild swelling was noted at the distal interphalangeal joint as well as at the tip of the affected finger. After appropriate analgesia was initiated, the child was sent to the Radiology department for X-ray imaging. The images obtained by the department are shown below in Figures 1.1 and 1.2.


Findings
Due to the lack of ideal positioning and suboptimal cooperation from the child and his parent, the radiology technician reports back to you stating that the best images they could obtain were the ones displayed above. Although unclear, you can confidently identify a small break in the bone at the base of the distal phalanx. You mention to the father that you see a fracture on the X-ray and report back to your Attending Physician.
The Attending Physician decides to take a break from his morning coffee and utters the dreaded question: “What kind of fracture is this?” You try to recall a lecture you had about Salter-Harris fractures but cannot recall the classification of these fractures. As if on cue, the father of the patient finds you shuffling your weight in front of the Attending Physician and asks: “You said he has a fracture, will he have to get surgery for his finger?”

Salter-Harris Fractures
Salter-Harris Fractures refer to fractures that involve the growth plate (physis). Therefore, these fractures are applicable specifically to the pediatric population, occurring most often during periods of rapid growth (growth spurts) when the growth plate is at its weakest, close to age ranges where children tend to participate in high-risk activities (11-12 in girls and 12-14 in boys) [1].
Originally described in 1963 by Dr Robert Salter and Dr Robert Harris [2], the now infamous Salter-Harris fractures are classified by the region of bone that is affected. Figure 2 displays the gross anatomy of a normal distal phalanx similar to the picture we examined in the X-ray, labelled to reflect the different areas of the bone relative to each other. The types of fractures that can occur are outlined below.

-
Type I Salter-Harris Fractures (Slipped)
Type I fractures occur when a longitudinal force is applied across the physis, resulting in a displacement (“slip”) of the epiphysis from the metaphysis. Though relatively infrequent (5%), suspicion of this fracture is raised when the epiphysis is seen to either be displaced to the side of its original position relative to the metaphysis or when the gap between the two segments is widened.

-
Type II Salter-Harris Fractures (Above)
Type II fractures are the most common (75%) of the Salter-Harris fractures. As with our patient above, this fracture only involves structures “Above” the epiphysis (Metaphysis + Physis/growth plate) with virtually no fracture or displacement of the epiphysis itself. Fortunately, type I and most type II fractures can be managed conservatively with cast immobilization and splinting.

-
Type III Salter-Harris Fractures (Lower)
Type III fractures involve both the physis and the epiphysis. Although relatively uncommon (10%), the involvement of the epiphysis and consequent disruption of the growth plate makes this an intra-articular fracture that usually requires surgical fixation.

-
Type IV Salter-Harris Fractures (Through)
Continuing the trend of worse outcomes with higher classification types, Type IV fractures involve all three layers (metaphysis, physis and epiphysis) and thus harbor more adverse outcomes and risks, with management primarily consisting of operative internal fixation. Similar to Type III fractures, this is an intra-articular fracture and also occurs at a similar rate of 10%.

-
Type V Salter-Harris Fractures (Rammed/Crushed)
The rarest of all the Salter-Harris fractures, type V fractures occur due to high impact compression of the growth plate. Potential disruption of the germinal matrix and compromised vascular supply to the growth plate can lead to growth arrest.

A convenient method to recall the Salter-Harris classifications is outlined below using the mnemonic “SALTR”

Case Resolution
You ascertain the patient’s fracture to be a type II Salter-Harris fracture, justifying your answer to the Attending Physician by pointing out that the affected region in the X-ray is limited to the metaphysis and physis with no epiphyseal involvement. Recognizing the potential for parental misconceptions surrounding the diagnosis of fractures in pediatric patients [3], you approach the father and explain that, though there is a fracture present, there is likely no need for any surgical intervention. You advise that the left index finger will be immobilized using a splint and further elaborate on the unlikelihood of this injury to manifest any long-term developmental or growth arrest in the affected region.
References and Further Reading
- Levine RH, Foris LA, Nezwek TA, et al. Salter Harris Fractures. [Updated 2019 Aug 13]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2019 Jan
- Salter, Robert B.; Harris, W. Robert: Injuries Involving the Epiphyseal Plate, The Journal of Bone and Joint Surgery (JBJS): April 1963 – Volume 45 – Issue 3 – p 587-622
- Sofu H, Gursu S, Kockara N, Issin A, Oner A, Camurcu Y. Pediatric fractures through the eyes of parents: an observational study. Medicine (Baltimore). 2015;94(2):e407. doi:10.1097/MD.0000000000000407
Sharing is caring
- Share on X (Opens in new window) X
- Share on Reddit (Opens in new window) Reddit
- Share on LinkedIn (Opens in new window) LinkedIn
- Share on Facebook (Opens in new window) Facebook
- Share on Tumblr (Opens in new window) Tumblr
- Share on Pinterest (Opens in new window) Pinterest
- Share on WhatsApp (Opens in new window) WhatsApp
- Email a link to a friend (Opens in new window) Email
- Print (Opens in new window) Print